







Content Menu
● Understanding Bronchoscope Technology
>> Basic Design and Components
● Historical Development and Technological Evolution
>> Modern Technological Advancements
>> Airway Inspection and Visualization
>> Airway Management and Intervention
>> Advanced Therapeutic Procedures
● Specialized Bronchoscope Procedures
>> Interventional Pulmonology Applications
● FAQ
>> 1. What is the difference between a flexible and rigid bronchoscope?
>> 2. What conditions typically require bronchoscopy?
>> 3. Is bronchoscopy a painful procedure?
>> 4. How long does a bronchoscopy procedure typically take?
>> 5. What are the risks associated with bronchoscopy?
A Bronchoscope represents one of the most essential tools in modern respiratory medicine, serving as a crucial instrument for visualizing the interior of the airways and performing various diagnostic and therapeutic procedures. This sophisticated medical device enables pulmonologists and other healthcare professionals to examine the tracheobronchial tree, obtain tissue samples, and perform interventions within the respiratory system. The development of Bronchoscope technology has revolutionized the diagnosis and treatment of pulmonary conditions, allowing for minimally invasive procedures that previously required thoracotomy or other surgical approaches. Understanding the fundamental aspects of the Bronchoscope, including its design, functionality, and applications, is essential for medical professionals involved in respiratory care.
The evolution of Bronchoscope technology spans more than a century, progressing from rigid metal tubes to sophisticated flexible fiberoptic and digital systems. Today's Bronchoscope incorporates advanced imaging technology, working channels for instrument passage, and deflection mechanisms that enable navigation through the complex branching structure of the bronchial tree. This comprehensive guide explores the various types of Bronchoscope instruments, their clinical applications, and the technological advancements that continue to expand their utility in respiratory medicine.

The fundamental architecture of a Bronchoscope consists of several integrated components that work together to provide visualization and access to the respiratory tract. A standard flexible Bronchoscope typically features an insertion tube ranging from 2.0 to 6.0 millimeters in diameter, containing fiberoptic bundles or digital imaging sensors, light transmission fibers, a working channel, and deflection control wires. The control section of the Bronchoscope houses the deflection controls, working channel port, and eyepiece or video connection, serving as the interface between the operator and the instrument. The distal tip of the Bronchoscope contains the imaging components, light sources, and working channel opening, all carefully arranged to maximize functionality within the confined spaces of the airways.
The working channel of a Bronchoscope represents one of its most important features, allowing passage of various instruments for diagnostic and therapeutic purposes. Depending on the Bronchoscope model, the working channel typically measures between 1.2 and 3.2 millimeters in diameter, accommodating biopsy forceps, needles, brushes, baskets, laser fibers, and other specialized instruments. The deflection mechanism of a flexible Bronchoscope enables the distal tip to bend in multiple directions, typically offering 180-220 degrees of upward deflection and 120-160 degrees of downward deflection. This controlled flexibility allows the Bronchoscope to navigate the branching architecture of the bronchial tree and access peripheral airways for comprehensive examination and intervention.
Modern respiratory medicine utilizes several distinct types of Bronchoscope instruments, each designed for specific clinical applications. The flexible Bronchoscope represents the most commonly used variant in contemporary practice, featuring a pliable shaft that can navigate the natural curvatures of the airway. This type of Bronchoscope is available in various diameters, with thinner models designed for pediatric use or examination of peripheral airways. The rigid Bronchoscope maintains an important role in specific therapeutic applications, featuring a straight metal tube that provides superior stability and larger working channels for managing significant bleeding, removing foreign bodies, or performing complex interventions.
Technological advancements have led to the development of specialized Bronchoscope systems with enhanced capabilities. The video Bronchoscope incorporates a digital image sensor at the distal tip, providing superior image quality compared to traditional fiberoptic models. Ultrathin Bronchoscope instruments with external diameters of less than 3 millimeters enable access to the most peripheral airways, expanding the diagnostic reach of bronchoscopic procedures. Recent innovations include disposable Bronchoscope systems that eliminate reprocessing requirements and reduce infection transmission risks. The diversity of Bronchoscope designs available today allows pulmonologists to select the most appropriate instrument for each clinical scenario, optimizing both diagnostic yield and therapeutic effectiveness.
The historical development of the Bronchoscope dates back to the late 19th century when German laryngologist Gustav Killian performed the first documented bronchoscopic procedure in 1897 using a rigid esophagoscope. The initial Bronchoscope designs were essentially rigid metal tubes equipped with a simple light source, allowing limited visualization of the central airways. American laryngologist Chevalier Jackson significantly advanced rigid Bronchoscope technology in the early 20th century, developing improved illumination systems and specialized instruments for foreign body removal. These early Bronchoscope systems established the foundation for endoscopic examination of the airways but were limited by their inability to access beyond the main bronchi.
The introduction of the flexible fiberoptic Bronchoscope in the 1960s represented a revolutionary advancement in respiratory endoscopy. Japanese innovator Shigeto Ikeda pioneered the development of the flexible Bronchoscope, recognizing the limitations of rigid instruments for examining the peripheral airways. The first flexible Bronchoscope utilized coherent fiberoptic bundles to transmit images from the distal tip to an eyepiece, allowing navigation through the branching bronchial tree. This innovation dramatically expanded the diagnostic capabilities of bronchoscopy, enabling visualization of segmental and subsegmental bronchi that were previously inaccessible. The flexible Bronchoscope quickly became an indispensable tool in pulmonary medicine, establishing new standards for airway evaluation and intervention.
The transition from fiberoptic to video Bronchoscope systems in recent decades has represented another significant technological leap in respiratory endoscopy. Modern video Bronchoscope instruments incorporate miniature charge-coupled device (CCD) or complementary metal-oxide-semiconductor (CMOS) sensors at the distal tip, providing high-resolution digital imaging that surpasses the quality of fiberoptic systems. This advancement in Bronchoscope technology has improved the detection of subtle mucosal abnormalities and enhanced procedural precision. The electronic platform of video Bronchoscope systems also facilitates integration with various imaging enhancements, such as narrow-band imaging and autofluorescence bronchoscopy.
Recent innovations in Bronchoscope technology continue to expand the capabilities of respiratory endoscopy. Ultrathin Bronchoscope models with external diameters of 2.8 millimeters or less enable navigation to the lung periphery, supporting the development of transbronchial biopsy techniques for peripheral pulmonary lesions. The incorporation of electromagnetic navigation technology with Bronchoscope systems has further enhanced the ability to reach and sample distant lung nodules. Robotic Bronchoscope platforms represent the latest advancement, offering improved stability and precision during complex endoscopic procedures. These continuous technological improvements ensure that the Bronchoscope remains at the forefront of minimally invasive pulmonary diagnosis and treatment.
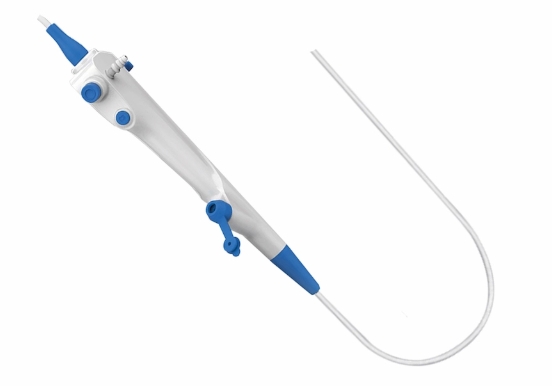
The fundamental diagnostic application of the Bronchoscope involves direct visualization of the tracheobronchial tree to identify structural abnormalities, inflammatory changes, and neoplastic lesions. Using a Bronchoscope, pulmonologists can systematically examine the airways from the vocal cords down to the subsegmental bronchi, assessing mucosal integrity, vascular pattern, and dynamic function during respiration. The magnified view provided by the Bronchoscope allows detection of subtle abnormalities that might not be apparent on radiographic studies, including early carcinomas, precancerous dysplasia, and inflammatory changes associated with various pulmonary diseases. This visual inspection capability makes the Bronchoscope an essential tool for evaluating patients with unexplained respiratory symptoms or abnormal imaging findings.
Advanced imaging modalities integrated into modern Bronchoscope systems enhance the detection of clinically significant pathology. Narrow-band imaging (NBI) utilizes specific light wavelengths to emphasize mucosal vascular patterns, improving the identification of dysplastic and neoplastic lesions that may appear normal under white-light examination. Autofluorescence Bronchoscope systems exploit the different fluorescence properties of normal and abnormal tissues, causing premalignant and malignant lesions to appear as dark areas against a green background. These enhanced visualization techniques significantly improve the diagnostic sensitivity of Bronchoscope examination for early lung cancer detection, particularly in high-risk populations.
The Bronchoscope enables various tissue sampling procedures that are essential for establishing histological diagnoses of pulmonary conditions. Bronchial biopsy through the Bronchoscope working channel allows direct sampling of endobronchial lesions under visual guidance, providing tissue for pathological examination. Transbronchial biopsy utilizes the Bronchoscope to guide forceps beyond visual range into the pulmonary parenchyma, obtaining samples of peripheral lung tissue for diagnosing interstitial lung diseases, infections, or malignancies. The precision of Bronchoscope-guided biopsy maximizes diagnostic yield while minimizing the risk of complications.
Beyond forceps biopsy, the Bronchoscope facilitates several other sampling techniques. Bronchial brushings obtained through the Bronchoscope provide cytological specimens from suspicious airway lesions, complementing histological samples from biopsy. Transbronchial needle aspiration (TBNA) performed with the Bronchoscope allows sampling of mediastinal and hilar lymph nodes through the bronchial wall, providing crucial staging information for lung cancer patients. Bronchoalveolar lavage (BAL) involves instilling sterile saline through the Bronchoscope into specific lung segments and then retrieving the fluid for microbiological, cytological, and immunological analysis. These diverse sampling capabilities make the Bronchoscope a versatile diagnostic platform for investigating various pulmonary disorders.
The Bronchoscope serves numerous therapeutic roles in managing airway disorders and complications. For patients with central airway obstruction from tumors, strictures, or foreign bodies, the Bronchoscope provides direct access for various interventional procedures. Through the working channel of the Bronchoscope, pulmonologists can deploy stents to maintain airway patency, use laser or electrocautery to debulk tumors, and apply cryotherapy or argon plasma coagulation to destroy abnormal tissue. The therapeutic Bronchoscope also facilitates balloon dilation of benign strictures and removal of aspirated foreign bodies using specialized retrieval devices. These interventions can provide immediate relief of respiratory symptoms and potentially be life-saving in cases of critical airway obstruction.
The management of massive hemoptysis represents another important therapeutic application of the Bronchoscope. In cases of significant pulmonary bleeding, the Bronchoscope allows identification of the bleeding source and targeted intervention to control hemorrhage. Through the Bronchoscope, operators can apply topical vasoconstrictors, use balloon tamponade to isolate bleeding segments, or deploy laser or electrocautery to coagulate bleeding sites. The rigid Bronchoscope is particularly valuable in massive hemoptysis, as its larger working channel facilitates suctioning of blood clots and maintenance of airway patency while interventions are performed. These therapeutic capabilities make the Bronchoscope an essential tool in the management of various airway emergencies.
The therapeutic applications of the Bronchoscope have expanded significantly with technological advancements, enabling increasingly complex interventions. Bronchoscopic lung volume reduction (BLVR) procedures use the Bronchoscope to deploy one-way valves or other devices in airways supplying emphysematous lung regions, causing selective collapse of hyperinflated areas and improving respiratory mechanics in selected COPD patients. For patients with severe asthma, bronchial thermoplasty delivered through the Bronchoscope applies controlled thermal energy to airway walls, reducing smooth muscle mass and decreasing bronchoconstriction.
The Bronchoscope also plays a crucial role in modern interventional pulmonology procedures for early-stage lung cancer. Bronchoscopic ablation techniques using photodynamic therapy, cryotherapy, or electrocautery delivered through the Bronchoscope can provide definitive treatment for superficial malignancies in patients who are not surgical candidates. The development of hybrid Bronchoscope systems that integrate with navigation platforms and real-time imaging technologies has further expanded the therapeutic potential of bronchoscopy, enabling precise targeting of peripheral lung lesions for localized treatment. These advanced applications demonstrate how the Bronchoscope has evolved from a purely diagnostic tool to a versatile platform for minimally invasive pulmonary interventions.
The field of interventional pulmonology has developed around advanced Bronchoscope procedures for diagnosing and treating complex thoracic conditions. Endobronchial ultrasound (EBUS) integrates ultrasonic technology with the Bronchoscope, allowing real-time imaging of structures beyond the airway walls. The EBUS Bronchoscope features an ultrasonic transducer at its distal tip that provides detailed visualization of mediastinal and hilar lymph nodes, enabling precise needle aspiration for lung cancer staging and diagnosis of other mediastinal pathologies. This Bronchoscope technology has revolutionized mediastinal evaluation, often eliminating the need for more invasive surgical procedures.
Electromagnetic navigation bronchoscopy (ENB) represents another advanced Bronchoscope application that combines bronchoscopy with virtual navigation technology. Using CT scan data to create a three-dimensional roadmap of the bronchial tree, the navigation Bronchoscope system guides operators to peripheral lung lesions that are beyond direct visualization. This Bronchoscope technology significantly improves the diagnostic yield for small peripheral nodules and enables targeted therapeutic interventions in the lung periphery. The continuous development of these specialized Bronchoscope procedures exemplifies how technological integration has expanded the capabilities of respiratory endoscopy beyond the limitations of conventional bronchoscopy.
In critical care settings, the Bronchoscope serves several essential functions for managing critically ill patients. For intubated patients in the intensive care unit, the Bronchoscope provides direct visualization during difficult intubations, guides proper positioning of endotracheal tubes, and facilitates timely diagnosis of ventilator-associated pneumonia through protected specimen brushing or BAL. The therapeutic Bronchoscope also enables management of atelectasis by directly suctioning mucus plugs and inspecting for other causes of lung collapse. In patients with tracheostomies, the Bronchoscope assists with tube changes, assesses for complications, and guides percutaneous dilatational tracheostomy procedures.
The diagnostic capabilities of the Bronchoscope are particularly valuable in immunocompromised patients with pulmonary infiltrates, where rapid identification of infectious agents or drug toxicity can significantly impact management decisions. In cases of suspected aspiration, the Bronchoscope allows direct assessment of airway injury and can guide therapeutic lavage when appropriate. The versatility of the Bronchoscope in addressing various diagnostic and therapeutic challenges makes it an indispensable tool in the critical care environment, where timely intervention can be life-saving for vulnerable patient populations.
The Bronchoscope has established itself as a cornerstone of modern respiratory medicine, with applications spanning diagnostic evaluation, therapeutic intervention, and critical care management. From its origins as a simple rigid tube for examining the central airways to the sophisticated digital systems of today, the Bronchoscope has continuously evolved to meet the expanding needs of pulmonary medicine. The technological advancements in Bronchoscope design, including improved imaging capabilities, enhanced flexibility, and integration with complementary technologies, have steadily pushed the boundaries of what can be achieved through minimally invasive airway procedures.
The future of Bronchoscope technology promises even greater capabilities, with ongoing developments in robotic assistance, molecular imaging, and therapeutic applications. As these innovations continue to emerge, the Bronchoscope will likely play an increasingly important role in the early detection and minimally invasive treatment of pulmonary diseases. The fundamental advantages of the Bronchoscope—its ability to provide direct visualization of the airways, facilitate tissue sampling, and perform therapeutic interventions through natural anatomical passages—ensure its continued central position in respiratory medicine. Understanding the full spectrum of Bronchoscope applications enables pulmonologists and other healthcare professionals to leverage this powerful technology effectively across the diverse range of conditions affecting the respiratory system.
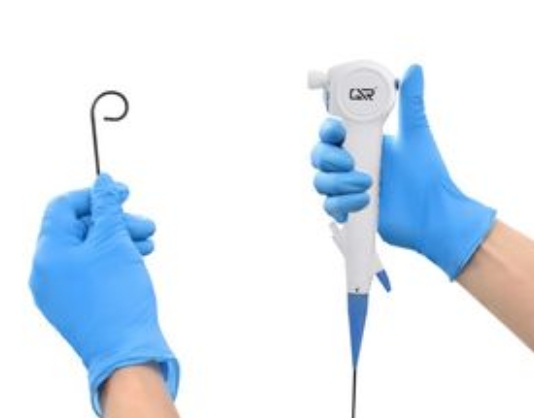
The primary difference between flexible and rigid Bronchoscope instruments lies in their design characteristics and clinical applications. The flexible Bronchoscope features a pliable shaft that can navigate the natural curvatures and branching structure of the bronchial tree, allowing examination from the trachea down to subsegmental bronchi. This type of Bronchoscope is typically used for diagnostic procedures, airway inspection, and sampling of peripheral lesions. In contrast, the rigid Bronchoscope consists of a straight metal tube that provides a stable conduit for the airway, enabling management of significant bleeding, removal of large foreign bodies, and performance of complex therapeutic interventions. The rigid Bronchoscope requires general anesthesia and offers superior suction capability and instrument passage compared to the flexible Bronchoscope.
Numerous pulmonary conditions may necessitate Bronchoscope evaluation and intervention. Diagnostic indications for Bronchoscope procedures include evaluation of persistent cough, hemoptysis (coughing up blood), unexplained wheezing, abnormal chest imaging findings, suspected lung cancer, and infectious processes requiring microbiological sampling. The Bronchoscope is also essential for assessing airway injury in inhalation trauma, evaluating suspected foreign body aspiration, and obtaining tissue diagnosis in interstitial lung diseases. Therapeutic applications of the Bronchoscope include management of central airway obstruction from tumors or strictures, removal of foreign bodies, control of massive hemoptysis, and treatment of early-stage lung cancer through various ablation techniques.
Bronchoscope procedures are typically performed under sedation or anesthesia to ensure patient comfort. Flexible Bronchoscope examinations are commonly done under conscious sedation, which induces a relaxed and drowsy state while maintaining patient cooperation. Most patients do not experience significant pain during Bronchoscope procedures, though they may feel pressure during scope insertion and have a strong urge to cough when the Bronchoscope passes through the vocal cords. Some discomfort may occur after the procedure, including sore throat, hoarseness, or minor blood-streaked sputum. Rigid Bronchoscope procedures require general anesthesia in an operating room setting, ensuring the patient experiences no discomfort during the examination.
The duration of a Bronchoscope procedure varies depending on its complexity and purpose. A simple diagnostic Bronchoscope examination for airway inspection may require only 15-30 minutes. More complex Bronchoscope procedures involving multiple biopsies, bronchoalveolar lavage, or peripheral navigation typically take 30-60 minutes. Advanced Bronchoscope interventions such as stent placement, tumor debulking, or electromagnetic navigation bronchoscopy may extend beyond 60 minutes. The total time commitment for patients includes pre-procedure preparation, the Bronchoscope examination itself, and recovery from sedation, typically amounting to 2-4 hours from arrival to discharge for outpatient procedures.
While Bronchoscope procedures are generally safe, they do carry potential risks that vary with the complexity of the procedure and patient factors. Common minor complications include sore throat, hoarseness, transient fever, and minor bleeding from biopsy sites. More significant risks associated with Bronchoscope procedures include respiratory depression from sedation medications, bronchospasm, laryngospasm, pneumothorax (particularly after transbronchial biopsy), significant bleeding, and infection. The overall complication rate for diagnostic Bronchoscope procedures is approximately 1-2%, with major complications occurring in less than 0.5% of cases. The risk-benefit ratio of Bronchoscope procedures is carefully considered for each patient, with precautions taken to minimize potential complications.
[1] https://www.brit-thoracic.org.uk/quality-imphttps://www.nature.com/articles/s41533-019-0127-9
[2] https://ccforum.biomedcentral.com/articles/10.1186/s13054-016-1577-x
[3] https://www.thoracic.org/professionals/clinical-resources/critical-care/clinical-education/bronchoscopy.php