Views: 222 Author: Lake Publish Time: 2025-11-05 Origin: Site








Content Menu
● Understanding the Bronchoscope and Its Types
● Diagnostic Applications of the Bronchoscope
● Therapeutic and Interventional Uses of the Bronchoscope
● The Bronchoscopy Procedure: What to Expect
>> Preparation for Bronchoscopy
>> Post-Procedure Care and Recovery
● Technological Advancements and the Future of Bronchoscopy
>> 1. What is the difference between a flexible and a rigid bronchoscope?
>> 2. How long does a bronchoscopy procedure take?
>> 3. Is a bronchoscopy painful?
>> 4. What are the most common risks associated with bronchoscopy?
>> 5. Can a bronchoscope be used to treat lung cancer?
In the rapidly advancing field of medical visualization, the bronchoscope stands as a critical tool for diagnosing and treating a wide range of pulmonary conditions. As a company deeply embedded in the development and OEM manufacturing of medical visualization devices, including endoscopy systems, disposable ureteroscopes, visual flexible laryngoscopes, bronchoscopy workstations, medical image processors, and video laryngoscopes, we recognize the transformative impact this technology has had on respiratory medicine. Essentially, a bronchoscope is a flexible or rigid tube equipped with a light source and camera that allows physicians to examine the airways and lungs in real-time. The primary purpose of a bronchoscope is to provide a direct, visual means of investigating the respiratory tract, enabling both diagnostic and therapeutic interventions without the need for invasive surgery.
The journey of the bronchoscope began decades ago with rigid models, which, while effective for certain procedures, limited the scope of exploration to the upper airways. The advent of the flexible bronchoscope revolutionized the field, permitting access to the deeper, more branching pathways of the lungs. Today, the bronchoscope is an indispensable instrument in pulmonology, critical for evaluating persistent coughs, unexplained lung shadows on X-rays, suspected tumors, and complex infections. Furthermore, the integration of a bronchoscope with advanced bronchoscopy workstations and medical image processors has enhanced its capabilities, allowing for precise navigation, detailed imaging, and sophisticated procedures.
This article delves into the multifaceted uses of the bronchoscope, exploring its role in modern medicine from diagnostic assessments to life-saving treatments. We will examine the different types of bronchoscope available, the detailed procedures involved, the latest technological advancements, and how our company's expertise in medical visualization and OEM services supports the global healthcare community in leveraging this vital technology. By understanding what a bronchoscope is used for, medical professionals and industry partners can better appreciate its value and applications.

A bronchoscope is an endoscopic device specifically designed for the examination of the interior of the airways and lungs. At its core, a bronchoscope consists of a long, thin tube that can be either flexible or rigid, equipped with a light source and a miniature camera at its tip. This camera transmits real-time images to a monitor, providing a clear view of the bronchial tree. The flexible bronchoscope is the most commonly used type today, particularly for diagnostic purposes, due to its ability to navigate the tortuous and narrow pathways of the lower respiratory system. Its construction typically involves fiber-optic bundles or a digital chip at the tip, which captures high-resolution images. The flexibility allows the bronchoscope to be passed through the nose or mouth, down the throat, between the vocal cords, and into the bronchi with relative ease and minimal patient discomfort.
In contrast, the rigid bronchoscope is a straight, hollow metal tube that is primarily used in therapeutic settings. It is indispensable for managing significant airway obstructions, removing large foreign bodies, controlling massive hemoptysis (lung bleeding), and placing airway stents. The rigid bronchoscope offers a larger working channel, superior suction capability, and better control in unstable airways, but it requires general anesthesia and is generally limited to the larger, more proximal airways. The choice between a flexible and rigid bronchoscope depends on the specific clinical scenario, with the flexible bronchoscope being the go-to for most diagnostic and many therapeutic procedures, while the rigid bronchoscope is reserved for more complex interventions.
The evolution of the bronchoscope has been significantly influenced by advancements in medical visualization technology. Modern bronchoscope systems are often part of an integrated bronchoscopy workstation that includes high-definition monitors, image processing units, and recording capabilities. These bronchoscopy workstations enhance the functionality of the bronchoscope by providing better image quality, storing procedural data, and facilitating complex interventions. Furthermore, the development of disposable bronchoscopes is gaining traction, reducing the risk of cross-contamination and eliminating the need for reprocessing. As an OEM service provider, our company supports the creation of customized bronchoscope solutions, including disposable ureteroscopes and visual flexible laryngoscopes, tailored to the specific needs of our clients and the patients they serve.
The bronchoscope is a fundamental tool for diagnosing a wide array of lung diseases and conditions. One of its primary diagnostic uses is the investigation of persistent cough, unexplained chest X-ray abnormalities, or suspected lung infections. When a patient presents with a cough that lasts for weeks or shows an abnormal shadow on a chest X-ray, a bronchoscope allows direct visualization of the airways to identify inflammation, tumors, or other pathologies. The bronchoscope can also be used to collect samples from the lungs, which is crucial for confirming diagnoses and guiding treatment.
- Sample Collection Techniques: The bronchoscope enables various sampling methods. During the procedure, physicians can advance instruments through the working channel of the bronchoscope to obtain tissue and fluid samples. Key techniques include:
- Bronchoalveolar Lavage (BAL): This involves instilling a small amount of saline solution through the bronchoscope into a specific area of the lung and then suctioning it back. The retrieved fluid contains cells, bacteria, and other substances from the lower airways and alveoli, which can be analyzed for infections, inflammatory conditions, or cancer .
- Biopsy (Endobronchial and Transbronchial): Using forceps passed through the bronchoscope, doctors can take tissue samples from the bronchial wall (endobronchial biopsy) or from the lung parenchyma (transbronchial biopsy). These biopsies are vital for diagnosing lung cancer, interstitial lung diseases, and other localized disorders .
- Brushing: A small brush is used to scrape cells from the airway lining for cytological examination, often to detect cancerous or pre-cancerous cells .
- Transbronchial Needle Aspiration (TBNA): A needle is passed through the bronchoscope to obtain samples from lymph nodes or masses adjacent to the airways, which is essential for lung cancer staging .
Another significant diagnostic application of the bronchoscope is in the early detection and staging of lung cancer. With the integration of advanced technologies like endobronchial ultrasound (EBUS), the bronchoscope can be used to visualize and sample lymph nodes within the chest without invasive surgery. An EBUS-bronchoscope has an ultrasonic probe at its tip that generates real-time images of the airway walls and surrounding structures, allowing for precise needle aspiration of lymph nodes to determine if cancer has spread . This has become the standard of care for mediastinal staging in lung cancer. Additionally, for suspicious peripheral lung nodules that are difficult to reach with a standard bronchoscope, navigation bronchoscopy systems have been developed. These systems use pre-procedural CT scans to create a virtual 3D map of the patient's airways. Using electromagnetic or virtual navigation, the bronchoscope can be guided along a planned path to reach lesions in the lung periphery, enabling biopsy with greater accuracy and reduced risk . This enhances the diagnostic yield of the bronchoscope for early cancer detection.
The bronchoscope is also pivotal in evaluating respiratory infections, especially in immunocompromised patients. By using the bronchoscope to perform BAL, physicians can identify specific pathogens causing pneumonia or opportunistic infections, allowing for targeted antimicrobial therapy. It is also used to assess airway damage in patients who have inhaled smoke or toxic gases, and to investigate the source of unexplained hemoptysis (coughing up blood) . In all these diagnostic roles, the bronchoscope provides invaluable information that is often unattainable through non-invasive methods.
Beyond diagnosis, the bronchoscope is a powerful therapeutic tool, enabling a range of minimally invasive procedures to treat various lung conditions. One of the most critical therapeutic applications of a bronchoscope is the removal of foreign bodies or obstructions from the airways. This is particularly common in pediatric cases but also occurs in adults. The rigid bronchoscope is often the instrument of choice for this purpose, as its wide lumen allows for the passage of specialized forceps, baskets, and other retrieval devices to grasp and extract large objects. However, flexible bronchoscopes can also be used with grasping tools to remove smaller foreign bodies. The bronchoscope not only facilitates removal but also allows for inspection of the airways to ensure no fragments remain and to assess for any trauma caused by the object.
The bronchoscope plays a vital role in managing central airway obstructions caused by tumors, strictures, or compression. Through the bronchoscope, physicians can perform several interventions to restore airway patency and improve breathing:
- Tumor Debulking and Ablation: Using tools like laser, electrocautery (argon plasma coagulation), or cryotherapy probes passed through the bronchoscope, tumors within the airways can be ablated, resected, or shrunk to relieve obstruction .
- Airway Stenting: When a malignant or benign stricture compresses the airway, a stent can be placed under bronchoscope guidance to keep the airway open. The bronchoscope is used to accurately position and deploy self-expanding metal or silicone stents .
- Balloon Dilation: For narrowed airway segments, a balloon can be inflated through the bronchoscope to dilate the stricture and improve airflow .
Another life-saving application of the bronchoscope is in controlling significant pulmonary hemorrhage (massive hemoptysis). In such critical situations, the bronchoscope is used to identify the bleeding site. Once located, therapeutic bronchoscope techniques can be employed, such as topical application of vasoconstrictive drugs, iced saline lavage, or balloon tamponade to stop the bleeding. The rigid bronchoscope is particularly advantageous in massive hemoptysis due to its superior suction capability and ability to maintain airway patency . Furthermore, the bronchoscope is used for assisting in difficult intubations and placing tracheal or bronchial tubes in critically ill patients who require mechanical ventilation. In the intensive care unit, a bronchoscope can provide direct visualization during endotracheal intubation, ensuring proper tube placement and reducing the risk of complications. It is also instrumental in performing therapeutic lavage for conditions like pulmonary alveolar proteinosis, where large volumes of saline are instilled and removed via the bronchoscope to wash out the alveolar spaces . The versatility of the bronchoscope in these therapeutic roles underscores its indispensability in modern interventional pulmonology.
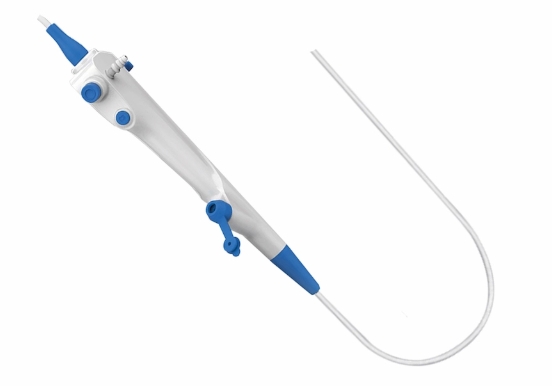
Understanding the bronchoscopy procedure is essential for both healthcare providers and patients. The process involving a bronchoscope is typically meticulous and follows a structured pathway to ensure safety and efficacy. The procedure with a bronchoscope usually takes place in a specialized room, such as an endoscopy suite, operating room, or intensive care unit, and is performed by a trained pulmonologist or surgeon. The entire process, from preparation to recovery, generally spans about four hours, though the actual examination with the bronchoscope itself often lasts between 30 to 60 minutes .
Proper preparation is crucial for a successful bronchoscope procedure. Patients are typically instructed to fast for at least 6 to 8 hours beforehand to prevent aspiration of stomach contents into the lungs . A thorough medical history review is conducted, and patients must inform their doctors of any medications, especially blood thinners like aspirin or warfarin, which may need to be temporarily discontinued to reduce the risk of bleeding . On the day of the procedure, patients are asked to remove dentures, hearing aids, or glasses and change into a hospital gown. As sedation is commonly used, arranging for someone to drive the patient home afterward is mandatory, as the effects of the sedatives can impair judgment and reflexes for several hours .
Once in the procedure room, the patient is positioned sitting up or lying on their back on an exam table. Monitors are attached to track heart rate, blood pressure, and oxygen levels throughout the bronchoscope examination . Sedative medications are administered through an intravenous line to help the patient relax and feel drowsy. It's important to note that patients are usually awake but sedated, able to breathe on their own and follow instructions if needed. A local anesthetic spray or gel is applied to the nose and throat to numb these areas and suppress the gag reflex, making the insertion of the bronchoscope more comfortable . The bronchoscope is then gently inserted through the nose or mouth, down the throat, past the vocal cords, and into the trachea and bronchi. Patients might feel a sensation of pressure or mild discomfort and may cough initially, but this usually subsides. The physician carefully advances the bronchoscope while watching the real-time video feed on a monitor. If necessary, instruments are passed through the working channel of the bronchoscope to collect samples or perform treatments. Throughout the procedure, the medical team ensures the patient's comfort and safety, adjusting oxygen levels as needed.
After the bronchoscope is removed, the patient is moved to a recovery area for observation for a few hours. The effects of the sedative wear off gradually, and the throat numbness may persist for one to two hours. During this time, patients are not allowed to eat or drink until the gag reflex returns to prevent choking . Once swallowing is safe, they can start with sips of water and then progress to soft foods. It's common to experience a sore throat, hoarseness, or a minor cough for a day or two; these symptoms can often be soothed with lozenges or gargling with warm water . If a biopsy was taken, slight blood-tinged sputum is normal. However, medical attention should be sought immediately if the patient develops a persistent fever, worsening chest pain, significant breathing difficulties, or coughs up more than a few tablespoons of blood . Most patients can resume normal activities the next day, and the doctor will discuss the initial findings within a few days, though biopsy results may take longer.
The field of bronchoscopy has witnessed remarkable technological evolution, significantly enhancing the capabilities of the bronchoscope. Navigation bronchoscopy represents a major leap forward, particularly for diagnosing peripheral lung lesions. Systems like Electromagnetic Navigation Bronchoscopy (ENB) use pre-procedural CT scans to create a virtual 3D roadmap of the patient's lungs. During the procedure, a sensor-equipped bronchoscope or locatable guide is tracked in real-time within an electromagnetic field, allowing the physician to navigate through the complex bronchial tree to reach distant targets with precision . This technology, often described as a "GPS for the lungs," has dramatically improved the diagnostic yield of bronchoscope-guided biopsies for small or hard-to-reach nodules, potentially enabling earlier diagnosis of lung cancer.
The integration of robotic technology with the bronchoscope is another groundbreaking development. Robotic bronchoscopy systems offer enhanced stability, greater maneuverability, and improved precision when navigating the bronchoscope to peripheral lesions. These systems often provide a degree of automation and stability that surpasses manual control, potentially leading to higher diagnostic accuracy and reduced procedure times. As these robotic bronchoscope platforms continue to evolve, they are expected to become more integrated with other imaging modalities and therapeutic capabilities. Furthermore, the trend towards miniaturization and disposable scopes is gaining momentum. Single-use, disposable bronchoscope models eliminate the risk of cross-infection and the logistical challenges of reprocessing, making them attractive for use in sterile environments or during infectious disease outbreaks. For OEM partners, this shift opens opportunities for designing and manufacturing specialized disposable bronchoscope units that are cost-effective and reliable.
The fusion of molecular imaging and advanced visualization is also shaping the future of the bronchoscope. Techniques like laser confocal microscopy and optical coherence tomography, which can be performed through a bronchoscope, provide microscopic-level images of the airway mucosa, allowing for in vivo histology. Additionally, the combination of a bronchoscope with real-time image processing and artificial intelligence (AI) is on the horizon. AI algorithms can assist in lesion detection, path planning, and even automated navigation of the bronchoscope, making procedures faster and more accurate. As a company at the forefront of medical visualization, we are actively involved in developing next-generation bronchoscopy workstations and image processors that integrate these advancements, providing our OEM clients with state-of-the-art solutions for pulmonary care.
The bronchoscope has firmly established itself as an indispensable tool in the arsenal of modern medicine, serving a dual role as both a diagnostic powerhouse and a therapeutic lifeline. From its fundamental use in visualizing airways and collecting crucial tissue samples to its advanced applications in navigating the lung's periphery and placing life-saving stents, the bronchoscope has transformed the management of pulmonary diseases. The ongoing technological evolution, including navigation systems, robotic assistance, and enhanced visualization, continues to expand the boundaries of what is possible with a bronchoscope, pushing towards earlier diagnoses, more precise treatments, and improved patient outcomes.
For medical professionals and industry partners, understanding the full scope of the bronchoscope's capabilities is key to leveraging its potential fully. As a specialist in medical visualization and OEM services, our company is committed to advancing bronchoscope technology and supporting the development of customized, high-quality devices that meet the evolving needs of the global healthcare market. Through continued innovation and collaboration, the bronchoscope will undoubtedly remain at the forefront of respiratory care, offering hope and healing to patients worldwide.
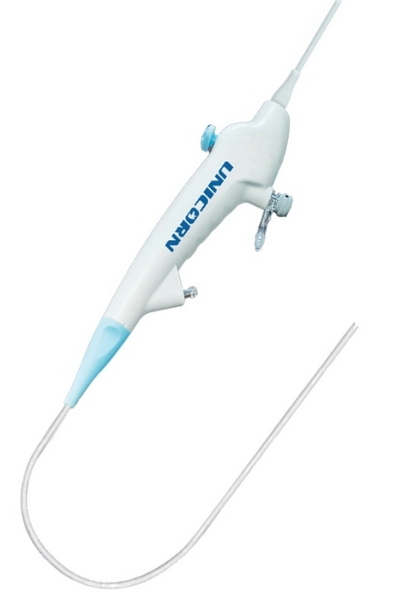
A flexible bronchoscope is a thin, bendable tube used for most diagnostic and many therapeutic procedures. It can navigate deep into the smaller airways and is typically performed under sedation with local anesthesia. In contrast, a rigid bronchoscope is a straight, metal tube used primarily for complex therapeutic interventions, such as removing large foreign bodies, controlling massive bleeding, or placing stents. It requires general anesthesia and provides a larger working channel for more substantial instruments .
The entire process, including preparation and recovery, usually takes about four hours. However, the actual examination with the bronchoscope typically lasts between 30 to 60 minutes, depending on the complexity of the procedure and whether additional interventions like biopsies or lavage are performed .
Patients are usually given sedatives to help them relax and local anesthesia to numb the throat and nose, so they should not feel pain during the procedure. There may be a sensation of pressure, a desire to cough, or mild discomfort as the bronchoscope passes through the throat, but this is generally well-tolerated. After the procedure, a sore throat or hoarseness is common but temporary .
Bronchoscopy is generally a safe procedure. The most common risks include minor bleeding (especially if a biopsy is taken), fever, and a sore throat. A less common but more serious risk is a pneumothorax (collapsed lung), which may occur if a lung biopsy is performed. Other rare complications include reactions to sedatives or anesthesia and infections .
Yes, a bronchoscope is used both in diagnosing and staging lung cancer through biopsies and EBUS, and also in treating certain aspects of the disease. Therapeutically, a bronchoscope can be used to debulk or ablate tumors obstructing the airways using lasers, electrocautery, or cryotherapy. It can also be used to place stents to keep airways open that are compressed by tumors, providing significant symptomatic relief .
[1]https://www.mayoclinic.org/zh-hans/tests-procedures/bronchoscopy/about/pac-20384746
[2]https://www.msdmanuals.cn/home/multimedia/video/navigational-bronchoscopy
[3]http://www.711hospital.com/Html/News/Articles/2352.html