Views: 222 Author: Lake Publish Time: 2025-11-07 Origin: Site








Content Menu
● Understanding Isolation Gowns
>> Definition and Basic Characteristics
>> Historical Development of Isolation Gowns
● Primary Uses of Isolation Gowns
>> Non-Healthcare Applications
>>> Laboratory and Research Settings
>>> Industrial and Environmental Applications
● Types and Classification of Isolation Gowns
>> Material Composition and Design Features
● Selection and Appropriate Use of Isolation Gowns
>> Risk Assessment and Gown Selection
>> Proper Donning and Doffing Procedures
● Specialized Applications and Considerations
>> Isolation Gowns in Pandemic Response
>> Environmental and Economic Considerations
>> 1. What is the difference between isolation gowns and surgical gowns?
>> 2. Can isolation gowns be reused?
>> 3. What level of isolation gown is appropriate for COVID-19 patient care?
>> 4. How should isolation gowns be disposed of after use?
>> 5. Are there alternatives when isolation gowns are not available?
Isolation gowns represent a critical component of personal protective equipment (PPE) in various settings, serving as essential barriers against contamination and infection transmission. These specialized garments have gained unprecedented visibility during global health crises, particularly the COVID-19 pandemic, where their importance in infection control protocols became widely recognized. Understanding what isolation gowns are used for extends beyond mere recognition of their existence to appreciating their multifaceted roles in protecting both wearers and others from hazardous materials. This comprehensive article explores the diverse applications, types, and significance of isolation gowns across different environments.
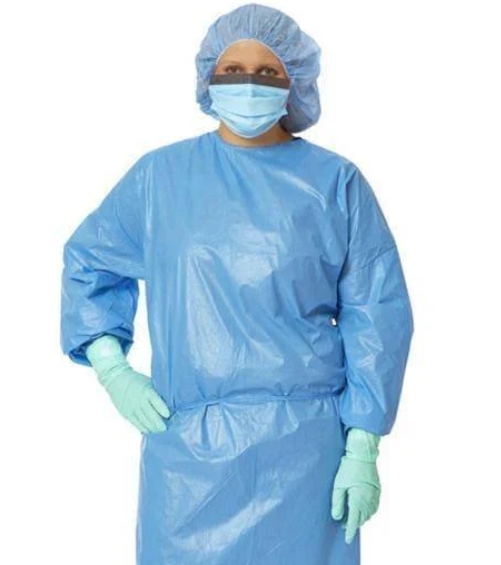
An isolation gown is a protective garment designed to shield the wearer's skin and clothing from potentially infectious materials, including microorganisms, bodily fluids, and other contaminants. Typically constructed from fluid-resistant materials, the isolation gown covers the torso from neck to knees and the arms from shoulder to wrist. The fundamental purpose of the isolation gown revolves around creating a reliable barrier that minimizes cross-contamination risks in situations where exposure to pathogens or hazardous substances is possible. While commonly associated with healthcare settings, the applications of isolation gowns extend to numerous other fields where protection from contamination is necessary.

An isolation gown is a protective garment intended to be worn over personal clothing to prevent the transfer of infectious materials and other contaminants. Unlike surgical gowns, which are sterile and used specifically in operative settings, isolation gowns are generally non-sterile and employed for isolation precautions in various scenarios. The typical isolation gown features long sleeves, a open-back design with tie closures, and sufficient length to provide coverage from the neck to below the knees. The materials used in manufacturing isolation gowns vary according to the intended application and required protection level, ranging from basic non-woven fabrics to sophisticated laminated materials with enhanced fluid resistance.
The design of an isolation gown prioritizes both protection and practicality. The garment must provide adequate barrier properties while allowing sufficient mobility for the wearer to perform necessary tasks. Modern isolation gowns often incorporate features such as elastic cuffs, reinforced critical zones, and various closure systems to enhance their protective capabilities. Understanding these basic characteristics helps clarify what isolation gowns are used for and how they differ from other types of protective apparel. The isolation gown serves as a customizable protective tool that can be selected according to specific risk assessments and task requirements.
The concept of protective garments in healthcare dates back centuries, with early references to covering garments used during plague outbreaks. However, the modern isolation gown as we know it today began to take shape in the late 19th and early 20th centuries with growing understanding of germ theory and infection transmission. Initially, isolation gowns were simple cloth garments that were laundered and reused, offering basic protection primarily for the wearer's clothing. The development of disposable materials in the mid-20th century revolutionized isolation gown technology, allowing for improved barrier properties and reduced cross-contamination risks.
The evolution of isolation gowns accelerated during the HIV/AIDS epidemic in the 1980s, which heightened awareness of bloodborne pathogen transmission and necessitated better protective standards. This period saw the implementation of standardized testing methods and classification systems for isolation gowns, particularly through the Association for the Advancement of Medical Instrumentation (AAMI) guidelines. More recently, the COVID-19 pandemic triggered unprecedented global demand for isolation gowns and highlighted their critical role in comprehensive infection control strategies [1]. The historical trajectory of isolation gown development demonstrates how changing understanding of disease transmission and technological advancements have shaped contemporary isolation gown design and usage protocols.
In healthcare environments, isolation gowns serve as essential protective barriers during patient care activities. The isolation gown is routinely used when there is anticipated contact with blood, bodily fluids, secretions, excretions, or contaminated environmental surfaces. Healthcare providers don an isolation gown before entering the room of patients on contact precautions, such as those with infectious diseases transmitted through direct or indirect contact. The isolation gown protects the healthcare worker's skin and clothing from contamination while also preventing the transfer of microorganisms from the provider to vulnerable patients.
Specific clinical situations requiring isolation gown use include dressing changes with excessive drainage, wound care procedures, and managing patients with incontinence or diarrhea. The isolation gown is also indispensable when caring for patients with multidrug-resistant organisms or those on contact isolation for pathogens like C. difficile norovirus. In these scenarios, the isolation gown acts as a removable barrier that can be discarded after use, reducing the risk of cross-contamination between patients and healthcare environments. Understanding what isolation gowns are used for in direct patient care highlights their role in breaking chains of infection transmission in clinical settings.
Beyond routine patient care, isolation gowns find important applications in various medical procedures where fluid exposure is possible but sterile conditions are not required. For instance, during peripheral intravenous insertion, urinary catheterization, or gastrointestinal procedures, an isolation gown provides protection against unexpected fluid exposure. While surgical procedures typically require sterile surgical gowns, many minor procedures and diagnostic tests utilize isolation gowns as practical protective barriers.
The isolation gown is particularly valuable in emergency departments, where healthcare providers may encounter patients with unknown infection status and potential exposure to bodily fluids. In these fast-paced environments, the isolation gown offers efficient protection that can be quickly donned when urgent situations arise. Additionally, isolation gowns are used in procedural areas such as endoscopy suites, radiology departments, and dialysis units, where contact with bodily fluids or contaminated equipment is possible. These applications demonstrate the versatility of the isolation gown as a protective tool across diverse healthcare scenarios.
Isolation gowns play crucial roles in laboratory environments where workers handle biological specimens, chemicals, or other hazardous materials. In microbiology laboratories, personnel routinely wear isolation gowns when processing clinical specimens to protect against accidental spills or splashes. The isolation gown serves as a primary barrier against potential pathogens present in patient samples, reducing exposure risks for laboratory staff. Similarly, in research laboratories working with infectious agents or hazardous substances, the isolation gown provides essential protection for personnel and helps maintain containment standards.
The specific requirements for isolation gowns in laboratory settings vary according to the biosafety level and procedures being performed. In higher containment laboratories (BSL-3 and BSL-4), isolation gowns may be supplemented with additional protective equipment or incorporated into more comprehensive protective systems. The isolation gown in these environments represents one component of a multi-layered approach to laboratory safety, working in conjunction with other controls to protect workers and maintain research integrity. Understanding what isolation gowns are used for in laboratory contexts underscores their importance beyond traditional healthcare applications.
Beyond medical and scientific fields, isolation gowns find applications in various industrial settings where protection from contaminants is necessary. In pharmaceutical manufacturing, cleanroom personnel often wear isolation gowns to maintain product purity and protect workers from potent compounds. The isolation gown in these environments helps control particulate contamination and prevents cross-contamination between different production areas. Similarly, in the electronics industry, workers may use specialized isolation gowns in cleanroom environments to prevent microscopic contamination during manufacturing processes.
Isolation gowns also serve important functions in environmental cleanup operations, particularly when dealing with hazardous materials or contaminated sites. Workers addressing chemical spills, biological hazards, or other environmental contaminants may utilize isolation gowns as part of their protective ensemble. In these applications, the isolation gown provides a disposable barrier that can be discarded after use, reducing the risk of carrying contaminants away from the worksite. These diverse industrial and environmental applications demonstrate the broad utility of isolation gowns beyond their traditional medical uses.
Isolation gowns are classified according to a standardized system developed by the Association for the Advancement of Medical Instrumentation (AAMI), which categorizes them based on their liquid barrier performance. The AAMI PB70 standard establishes four distinct levels of protection for isolation gowns:
- Level 1 Isolation Gown: This lowest protection level isolation gown is designed for minimal risk situations, with tested resistance to water only. The Level 1 isolation gown is appropriate for basic care or standard isolation where no fluid exposure is anticipated.
- Level 2 Isolation Gown: Providing low barrier protection, this isolation gown is suitable for situations where low fluid exposure is expected. The Level 2 isolation gown offers greater protection than Level 1 and is commonly used in routine patient care.
- Level 3 Isolation Gown: Offering moderate barrier protection, this isolation gown is appropriate for situations with moderate fluid exposure risks. The Level 3 isolation gown is frequently used during procedures with higher potential for fluid contact.
- Level 4 Isolation Gown: Delivering the highest level of protection, this isolation gown is designed for situations with high fluid exposure risks. The Level 4 isolation gown is essentially impermeable and used for high-risk procedures.
Understanding these classification levels is essential for selecting the appropriate isolation gown for specific tasks and exposure risks. The selection of an isolation gown should be based on a thorough risk assessment that considers the anticipated type and volume of fluid exposure, rather than automatically choosing the highest available protection level.
Isolation gowns are manufactured from various materials, each offering different characteristics in terms of protection, comfort, and environmental impact. Disposable isolation gowns are typically made from non-woven materials such as polypropylene, polyethylene, or SMS (spunbond-meltblown-spunbond) fabric. These materials provide effective barrier properties while remaining lightweight and breathable. The specific construction of the isolation gown material determines its fluid resistance, tensile strength, and comfort during extended wear.
Reusable isolation gowns are typically made from woven fabrics, often cotton or cotton-polyester blends, that undergo special finishing treatments to enhance their fluid-resistant properties. These isolation gowns can be laundered and reused multiple times, potentially offering economic and environmental advantages over disposable options. However, reusable isolation gowns require proper laundering procedures to maintain their protective qualities and prevent cross-contamination.
Design features of isolation gowns vary to accommodate different applications and user preferences. These may include different closure systems (tie-back, snap-fastened, or zip-front), varying sleeve designs (set-in or raglan), and specialized features such as thumb loops or reinforced areas. The design of an isolation gown influences its protective capabilities, donning and doffing ease, and overall functionality in specific use scenarios.
Selecting the appropriate isolation gown requires careful consideration of the specific task, anticipated exposure risks, and the desired balance between protection and practicality. A proper risk assessment should guide the selection process, considering factors such as the type of exposure anticipated (splash, spray, or large-volume fluid contact), the potential pathogens involved, and the duration of exposure. This assessment helps determine the required protection level and features needed in an isolation gown for each specific situation.
In healthcare settings, isolation gown selection is often guided by transmission-based precautions and specific procedure requirements. For standard precautions involving minimal fluid exposure, a Level 1 or 2 isolation gown may be sufficient. For contact precautions with patients known or suspected to have epidemiologically important pathogens, a higher-level isolation gown (Level 2 or 3) is typically recommended. During procedures with anticipated substantial fluid exposure, a Level 3 or 4 isolation gown provides appropriate protection. This risk-based approach to isolation gown selection ensures adequate protection while avoiding unnecessary use of high-level gowns that may be less comfortable or more costly.
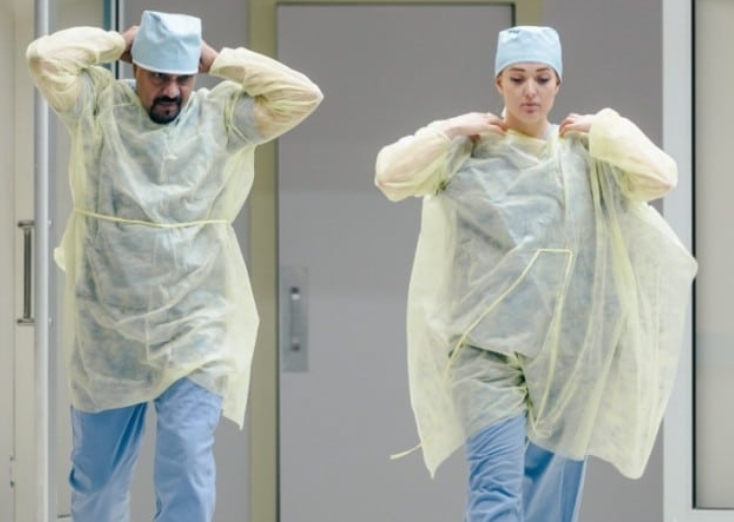
The protective effectiveness of an isolation gown depends not only on its quality and appropriate selection but also on correct donning and doffing techniques. Proper donning of an isolation gown begins with hand hygiene and inspection of the gown for any visible defects. The isolation gown should be unfolded carefully and donned by inserting arms into the sleeves, ensuring complete coverage of the torso and arms. The gown should then be secured at the neck and waist, with gloves donned last to cover the cuffs of the isolation gown.
Doffing (removing) the isolation gown requires equal care to avoid self-contamination. The removal process typically begins with glove removal followed by hand hygiene. The isolation gown is then untied or unfastened and removed by pulling it away from the body, turning it inside out during removal to contain contaminated surfaces. The used isolation gown should be disposed of properly according to institutional protocols, followed by another performance of hand hygiene. These meticulous procedures maximize the protective benefits of the isolation gown and minimize the risk of contamination during removal.
The COVID-19 pandemic highlighted the critical importance of isolation gowns in large-scale infectious disease response. During the pandemic, isolation gowns became essential PPE for healthcare workers managing COVID-19 patients, particularly in settings where contact with respiratory secretions or contaminated surfaces was likely. The massive global demand for isolation gowns during this period strained supply chains, leading to shortages that necessitated conservation strategies and emergency use authorizations for alternative products [2].
The pandemic experience underscored several aspects of isolation gown usage in crisis situations. First, it demonstrated the need for clear guidelines on appropriate isolation gown selection and use during emerging infectious disease outbreaks. Second, it highlighted the importance of maintaining adequate stockpiles of isolation gowns and other PPE for emergency preparedness. Third, it stimulated innovation in isolation gown design and manufacturing, including the development of reusable options and gowns made from alternative materials. These lessons from pandemic response continue to inform current practices and preparedness planning for isolation gown usage.
The widespread use of isolation gowns, particularly disposable models, raises important environmental and economic considerations. Disposable isolation gowns contribute to medical waste streams, creating disposal challenges and environmental impacts. The manufacturing processes for disposable isolation gowns also consume resources and energy, adding to their environmental footprint. These concerns have stimulated interest in sustainable alternatives, including reusable isolation gowns and disposable gowns made from biodegradable or recycled materials.
Economic factors also influence isolation gown selection and usage patterns. While disposable isolation gowns eliminate laundering costs, they require continuous repurchasing. Reusable isolation gowns involve higher initial investment but may offer cost savings over time through multiple use cycles. The economic analysis of isolation gown options should consider not only purchase prices but also storage, distribution, and disposal costs. Balancing infection control requirements with environmental and economic considerations represents an ongoing challenge in isolation gown management across various sectors.
Isolation gowns serve as vital protective barriers in numerous settings, primarily preventing the transmission of infectious materials and other hazardous substances. Understanding what isolation gowns are used for encompasses appreciating their roles in healthcare delivery, laboratory work, industrial applications, and emergency response. The appropriate selection and use of isolation gowns, guided by risk assessment and standardized classification systems, ensures effective protection while promoting efficient resource utilization.
The evolution of isolation gown technology continues to address changing needs in infection control and worker protection, with ongoing developments in materials, design, and sustainability. As global health challenges emerge and awareness of safety protocols grows, the importance of proper isolation gown usage remains paramount. By comprehending the diverse applications and proper implementation of isolation gowns, professionals across various fields can enhance safety standards and contribute to comprehensive risk management strategies. The isolation gown, though seemingly simple, represents a sophisticated tool in the ongoing effort to control infection transmission and protect both workers and vulnerable populations.
Isolation gowns and surgical gowns serve different purposes despite their similar appearance. An isolation gown is primarily used for isolation precautions in patient care situations where contact with bodily fluids, secretions, or excretions is anticipated. Isolation gowns are generally non-sterile and provide coverage primarily in the front, with varying back coverage depending on design. In contrast, surgical gowns are sterile garments designed specifically for use in surgical procedures, where they must provide a critical barrier against pathogen migration in both front and back areas during sterile operations. Surgical gowns undergo more rigorous testing for liquid barrier performance and are classified as Class II medical devices requiring FDA approval.
The reusability of an isolation gown depends on its type and manufacturer specifications. Disposable isolation gowns are designed for single use only and should not be reused, as their protective barriers may become compromised during use. Reusable isolation gowns, typically made from woven fabrics with fluid-resistant finishes, can be laundered and reused according to manufacturer instructions. Proper laundering of reusable isolation gowns is essential to maintain their protective qualities, including specific wash cycles, detergent types, and drying parameters. During supply shortages, some facilities may implement extended use protocols for disposable isolation gowns, but these are exceptional circumstances requiring specific risk assessments.
For COVID-19 patient care, the appropriate isolation gown level depends on the specific procedures being performed and the anticipated exposure risk. The Centers for Disease Control and Prevention (CDC) recommends using a gown that is rated at least Level 2 for routine care of COVID-19 patients, providing protection against low to moderate fluid exposure [2]. For procedures with higher fluid exposure risks, such as aerosol-generating procedures or situations with potential for substantial fluid contact, a Level 3 isolation gown is recommended. The selection should be based on a risk assessment considering the specific task, potential exposure to respiratory secretions, and other bodily fluids.
The disposal method for isolation gowns depends on their classification and the setting in which they are used. In healthcare facilities, disposable isolation gowns used in routine patient care are typically considered medical waste and should be disposed of according to institutional protocols for non-hazardous medical waste. If the isolation gown is heavily soiled with blood or bodily fluids, it may require disposal as regulated medical waste. In non-healthcare settings or for home use, isolation gowns can generally be disposed of with regular trash unless local regulations specify otherwise. Always follow facility-specific guidelines and local regulations for proper disposal of used isolation gowns.
During supply shortages when isolation gowns are unavailable, the CDC provides guidance on contingency and crisis capacity strategies [2]. These may include using isolation gowns past their designated shelf life, using gowns approved under FDA Emergency Use Authorizations, or using disposable coveralls as alternatives. In crisis situations, reusable patient gowns or laundered cloth gowns may be used, though these options generally provide less protection than standard isolation gowns. When no gowns are available, the CDC recommends prioritizing gown use for high-contact patient care activities and using designated PPE for specific procedures. Any alternative approaches should be implemented according to official guidance and with careful consideration of protection levels required for specific tasks.
[1] World Health Organization. (2020). Rational use of personal protective equipment for coronavirus disease (COVID-19) and considerations during severe shortages. WHO Reference Number: WHO/2019-nCov/IPC_PPE_use/2020.3
[2] Centers for Disease Control and Prevention. (2020). Strategies for Optimizing the Supply of Isolation Gowns. Retrieved from CDC website.