Views: 222 Author: Lake Publish Time: 2025-11-13 Origin: Site








Content Menu
● Understanding Nephrolithiasis
>> Pathophysiology and Stone Types
● Ureteroscope Equipment and Technology
>> Patient Selection and Counseling
>> Preoperative Medical Optimization
● Ureteroscopic Technique for Nephrolithiasis
>> Stone Management and Lithotripsy
● Special Considerations and Advanced Techniques
>> Management of Large and Complex Stones
>> Pediatric and Special Populations
● Complications and Management
>> Postoperative Complications
● Postoperative Care and Follow-up
>> Immediate Postoperative Management
>> Long-term Follow-up and Prevention
● FAQ
>> 1. What types of kidney stones can be treated with a ureteroscope?
>> 2. How long does recovery typically take after a ureteroscope procedure?
>> 3. What are the advantages of using a ureteroscope compared to other stone treatments?
>> 4. Is a stent always necessary after a ureteroscope procedure?
>> 5. What are the success rates for ureteroscope treatment of kidney stones?
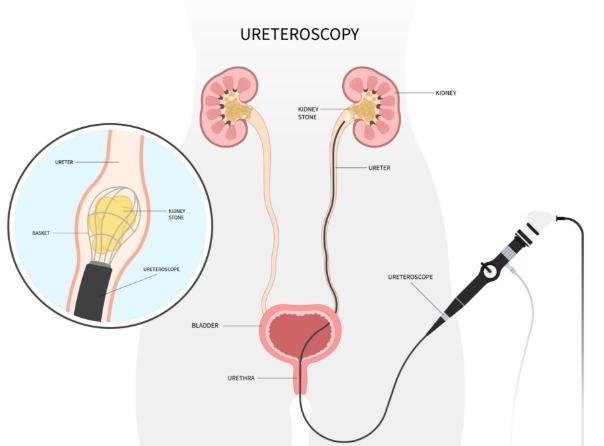
Nephrolithiasis, commonly known as kidney stones, represents a prevalent urological condition affecting millions worldwide. The ureteroscope has revolutionized the management of urinary tract stones, particularly those located in the upper ureter and kidneys. This minimally invasive approach has become the standard of care for many stone cases, offering significant advantages over traditional open surgical procedures. The evolution of ureteroscope technology, particularly with the advent of digital and flexible systems, has expanded the therapeutic possibilities for treating nephrolithiasis while minimizing patient discomfort and recovery time.
The modern ureteroscope represents a sophisticated medical instrument designed to navigate the intricate anatomy of the urinary tract while providing excellent visualization and therapeutic capabilities. Understanding the proper techniques for utilizing the ureteroscope in nephrolithiasis management requires knowledge of equipment selection, procedural steps, and postoperative care. This comprehensive guide examines the current approaches to ureteroscope-guided stone treatment, providing clinicians with detailed information to optimize patient outcomes in nephrolithiasis management.

Nephrolithiasis develops when crystalline compounds precipitate in the urine, forming solid structures within the renal collecting system. The composition of these stones significantly influences treatment decisions and approaches when using the ureteroscope. Calcium oxalate stones represent the most common variety, comprising approximately 70-80% of all urinary calculi. Struvite stones, associated with urinary tract infections, often form staghorn calculi that fill the renal pelvis and calyces. Uric acid stones, cysteine stones, and calcium phosphate stones constitute the remaining common stone types, each with distinct characteristics that may affect ureteroscope management strategies.
The location and size of stones play crucial roles in determining the appropriate treatment approach with the ureteroscope. Stones may be located in the renal calyces, renal pelvis, or various segments of the ureter. The ureteroscope provides access to stones throughout the urinary tract, though specific technical considerations apply to different locations. Understanding stone characteristics enables urologists to select the optimal ureteroscope approach, whether using rigid or flexible systems, and determine the appropriate lithotripsy method for stone fragmentation.
Comprehensive diagnostic evaluation precedes any ureteroscope procedure for nephrolithiasis. Non-contrast computed tomography (CT) of the abdomen and pelvis represents the gold standard for stone detection, providing detailed information about stone size, location, density, and urinary tract anatomy. This preoperative information guides the surgeon in planning the ureteroscope approach, selecting appropriate instruments, and anticipating potential challenges. Additional imaging studies, such as renal ultrasonography or intravenous pyelography, may provide complementary information in specific clinical scenarios.
Urinalysis and urine culture identify associated urinary tract infections that require treatment before ureteroscope intervention. Metabolic evaluation, including serum chemistry studies and 24-hour urine collection, helps identify underlying abnormalities contributing to stone formation. This comprehensive diagnostic approach ensures that ureteroscope treatment addresses not only the existing stones but also contributes to long-term management strategies to prevent recurrence. Proper patient selection for ureteroscope procedures based on these diagnostic findings optimizes therapeutic outcomes while minimizing complications.
The modern urologist has access to various ureteroscope designs, each with specific advantages for particular clinical situations. Rigid ureteroscope systems offer excellent irrigation flow and durability, making them ideal for stones in the distal and mid-ureter. These instruments typically feature a straight working channel that accommodates various lithotripsy probes and retrieval devices. The rigid ureteroscope provides superior stability during stone manipulation, though its limited flexibility restricts access to the proximal ureter and intrarenal collecting system.
Flexible ureteroscope technology has advanced significantly, enabling navigation through the tortuous ureter and into the renal collecting system. Modern digital flexible ureteroscope systems offer enhanced image quality, increased deflection capabilities, and improved durability compared to earlier fiberoptic models. The flexible ureteroscope has become indispensable for treating renal stones, particularly those located in lower pole calyces or other areas difficult to access with rigid instruments. The choice between rigid and flexible ureteroscope systems depends on stone location, surgeon preference, and available resources.
Successful ureteroscope stone management requires a complement of accessory instruments designed to work through the ureteroscope working channel. Lithotripsy devices include laser fibers, which have largely replaced earlier technologies such as electrohydraulic and pneumatic lithotripters. Holmium:YAG laser lithotripsy, delivered through flexible fibers that pass easily through the ureteroscope, effectively fragments stones of all compositions while minimizing tissue damage. The appropriate laser fiber size depends on the ureteroscope working channel diameter and the specific clinical situation.
Stone retrieval devices represent another essential category of ureteroscope accessories. Nitinol stone baskets come in various configurations designed for specific stone situations, from standard helical designs for capturing fragments to tipless versions that minimize mucosal trauma. Grasping forceps provide an alternative retrieval method, particularly for larger fragments. Access sheaths, while not passed through the ureteroscope, facilitate multiple entries into the ureter during flexible ureteroscope procedures, maintaining access while reducing intrarenal pressure and protecting the ureteroscope from damage.
Appropriate patient selection forms the foundation of successful ureteroscope management of nephrolithiasis. The ureteroscope approach proves most beneficial for stones between 5mm and 20mm in diameter, though technological advances have expanded the size range amenable to ureteroscope treatment. Proximal ureteral stones and renal stones, particularly those not responding to extracorporeal shock wave lithotripsy (ESWL), represent excellent indications for ureteroscope intervention. Patient factors such as anatomy, comorbidities, and stone characteristics all influence the decision to proceed with ureteroscope treatment.
Comprehensive patient counseling before ureteroscope procedures ensures realistic expectations and informed consent. Patients should understand the potential benefits of ureteroscope treatment, including high success rates, minimal invasiveness, and rapid recovery. They should also acknowledge possible complications such as infection, bleeding, ureteral injury, and the potential for additional procedures. Discussion of alternative treatments, including observation, medical expulsive therapy, ESWL, and percutaneous nephrolithotomy, provides context for the selected ureteroscope approach. This shared decision-making process promotes patient satisfaction and adherence to postoperative instructions.
Medical optimization before ureteroscope procedures reduces complication risks and improves outcomes. Identification and treatment of urinary tract infections represent a critical preoperative step, as untreated infection during ureteroscope intervention can lead to urosepsis. Preoperative urine culture guides antibiotic selection, with tailored antimicrobial prophylaxis administered before the ureteroscope procedure. Patients with complex medical conditions may require consultation with appropriate specialists to optimize their status before undergoing ureteroscope treatment.
Medication management forms another essential component of preoperative preparation for ureteroscope procedures. Anticoagulant and antiplatelet medications typically require temporary discontinuation before ureteroscope intervention, following consultation with the prescribing physician. Specific instructions regarding holding these medications depend on the specific agent and the patient's thrombotic risk. Clear communication between the urologist, patient, and other healthcare providers ensures safe medication management surrounding the ureteroscope procedure while minimizing both bleeding and thrombotic complications.
Successful ureteroscope stone treatment begins with careful access to the urinary tract. Cystoscopic examination precedes ureteroscope insertion, allowing assessment of the ureteral orifices and the bladder environment. Safety guidewire placement under fluoroscopic guidance establishes secure access to the upper urinary tract before ureteroscope introduction. The ureteroscope may be passed alongside the guidewire ("railroaded") or through an access sheath, depending on the specific clinical situation and surgeon preference.
Navigating the ureteroscope through the ureter requires gentle technique and constant visual guidance. The natural narrow points of the ureter, particularly the ureterovesical junction and the uretero pelvic junction, may present challenges during ureteroscope advancement. Hydrodilation with irrigation fluid or balloon dilation can facilitate ureteroscope passage when encountering resistance. Fluoroscopic monitoring complements endoscopic visualization during ureteroscope navigation, confirming position and identifying any anatomical variations. Patience and gentle technique during ureteroscope advancement minimize the risk of ureteral trauma and subsequent stricture formation.
Once the ureteroscope reaches the stone, systematic assessment guides the treatment approach. The ureteroscope provides magnified visualization of the stone and surrounding mucosa, allowing evaluation of stone size, impaction, and associated inflammation. Small stones may be retrieved intact with basket devices under ureteroscope guidance, while larger stones require fragmentation before removal. The holmium:YAG laser, applied through fibers passed through the ureteroscope working channel, represents the preferred lithotripsy method for most ureteroscope procedures.
Effective laser lithotripsy through the ureteroscope requires proper technique to optimize efficiency and safety. The laser fiber should extend sufficiently beyond the ureteroscope tip to prevent damage to the instrument while maintaining visualization. "Dusting" techniques using low energy and high frequency settings create fine particles that pass spontaneously, while "fragmentation" approaches produce larger pieces that require basket retrieval. The ureteroscope provides continuous visualization during lithotripsy, allowing adjustment of technique based on stone composition and behavior. Irrigation through the ureteroscope maintains visibility by clearing the field of stone dust and debris.
Systematic inspection of the entire collecting system with the ureteroscope ensures complete stone treatment before concluding the procedure. The ureteroscope should be withdrawn slowly while examining the ureteral mucosa for injury and confirming the absence of residual fragments. Small stone pieces may be flushed down the ureter with irrigation or retrieved with basket devices under ureteroscope visualization. The goal of ureteroscope treatment is complete stone clearance, though occasionally very small, non-obstructive fragments may be left in situ when further manipulation would increase risk.
The decision regarding postoperative drainage after ureteroscope procedures depends on several factors, including the extent of ureteral manipulation, presence of edema, and completeness of stone clearance. Ureteral stents provide drainage and prevent obstruction from edema, particularly after prolonged ureteroscope procedures or significant ureteral manipulation. Stentless ureteroscope procedures are increasingly common in selected patients, particularly those with minimal trauma and complete stone clearance. When placed, the stent string may be left for subsequent removal without a separate procedure, enhancing patient convenience after ureteroscope treatment.
The ureteroscope management of large renal stones requires specialized techniques and realistic expectations. Staged ureteroscope procedures may be necessary for complete clearance of large stone burdens, particularly when operating time or irrigation volume becomes concerning. The "dusting" technique, using laser settings that create fine particles, minimizes the need for fragment retrieval during ureteroscope procedures for large stones. Strategic fragmentation that produces pieces small enough to pass spontaneously yet large enough to avoid creating excessive dust represents an alternative ureteroscope approach.
The flexible ureteroscope has particular value for managing stones in anatomically challenging locations within the kidney. Lower pole stones traditionally presented difficulties for ureteroscope access, though modern highly deflecting ureteroscope systems and ancillary techniques such as patient positioning have improved success rates. Stones in calyceal diverticula may be effectively managed with ureteroscope techniques, often combined with laser incision of the diverticular neck. These advanced ureteroscope applications require experience and specialized equipment but offer minimally invasive alternatives to percutaneous approaches for complex stone situations.
Ureteroscope stone management in pediatric patients requires attention to unique anatomical considerations and specialized equipment. Pediatric ureteroscope systems with smaller diameters minimize trauma to the developing urinary tract while maintaining therapeutic capabilities. The principles of ureteroscope technique remain similar to adult procedures, though increased mucosal fragility and smaller caliber ureters demand heightened gentleness during ureteroscope manipulation. Successful ureteroscope outcomes in children require surgeons experienced with both the technique and the special considerations of pediatric urology.
Special populations requiring ureteroscope management include patients with anatomical variations such as urinary diversions, transplant kidneys, or duplicated systems. These situations often present technical challenges for ureteroscope access and navigation, frequently requiring customized approaches and creative problem-solving. Patients with bleeding diatheses or requiring continuous anticoagulation may benefit from ureteroscope treatment as a less invasive alternative to percutaneous procedures, though careful perioperative management remains essential. These complex scenarios highlight the versatility of the ureteroscope while emphasizing the need for individualized treatment planning.
Ureteroscope procedures, while minimally invasive, present potential intraoperative challenges that require prompt recognition and management. Difficult ureteroscope access may occur due to ureteral strictures, edema, or anatomical variations. Preoperative stenting, balloon dilation, or alternative access strategies may be necessary when the ureteroscope cannot be advanced safely. Ureteral perforation, though uncommon with careful ureteroscope technique, requires immediate recognition and often stent placement to promote healing while preventing urinoma formation.
Significant bleeding during ureteroscope procedures can obscure visualization and complicate stone treatment. Minor mucosal bleeding is common during ureteroscope manipulation, typically clearing with irrigation, but more substantial hemorrhage may require aborting the procedure and placing a stent. Proximal stone migration during ureteroscope lithotripsy represents another common challenge, particularly with upper ureteral stones. Prevention strategies include early basket stabilization, modified laser technique, or use of anti-retropulsion devices. These intraoperative challenges during ureteroscope procedures highlight the importance of experience, preparation, and adaptability.
Most patients experience rapid recovery after ureteroscope procedures, though certain postoperative complications require recognition and management. "Stent discomfort" represents the most common complaint after ureteroscope procedures, characterized by urinary frequency, urgency, and flank pain with voiding. Medical management with alpha-blockers, anticholinergics, or analgesics provides symptomatic relief until stent removal. Urinary tract infection may occur after ureteroscope procedures despite prophylactic antibiotics, requiring culture-directed treatment.
Steinstrasse, or "street of stones," describes the accumulation of fragments in the ureter causing obstruction after ureteroscope lithotripsy. This complication may require additional ureteroscope intervention or ESWL to relieve obstruction and clear fragments. Ureteral stricture represents a rare but serious late complication of ureteroscope procedures, typically resulting from significant ureteral trauma or ischemia. Regular follow-up after ureteroscope treatment identifies these complications early, allowing intervention before renal function compromise. Most ureteroscope complications resolve with appropriate management, particularly when recognized promptly.
The immediate postoperative period after ureteroscope procedures focuses on monitoring for complications and managing symptoms. Most ureteroscope procedures are performed outpatient, with discharge following recovery from anesthesia and successful voiding. Clear instructions regarding pain management, activity restrictions, and signs of complications ensure safe transition to home care. Patients with ureteral stents after ureteroscope procedures require specific education about stent symptoms and management strategies to minimize discomfort.
Medication management after ureteroscope procedures typically includes analgesics for discomfort and possibly medications to reduce stent-related symptoms. Alpha-blockers have demonstrated benefit in reducing stent discomfort and facilitating fragment passage after ureteroscope procedures. Continued antibiotics may be appropriate in selected cases, particularly when infection was present before the ureteroscope procedure or when prolonged stent placement is anticipated. This pharmacological management complements the mechanical stone treatment achieved with the ureteroscope, optimizing overall outcomes.
Systematic follow-up after ureteroscope procedures confirms treatment success and addresses stone prevention. Imaging, typically with renal ultrasonography or low-dose CT, assesses for residual fragments several weeks after ureteroscope treatment. The definition of success continues to evolve, with increasing acceptance of "clinically insignificant residual fragments" rather than insisting on absolute stone-free status after ureteroscope procedures. Metabolic evaluation identifies underlying abnormalities that contribute to stone formation, guiding preventive strategies that reduce recurrence risk beyond the ureteroscope treatment itself.
Lifestyle modifications and pharmacological interventions form the foundation of prevention after ureteroscope procedures. Increased fluid intake to maintain dilute urine represents the most effective preventive measure, reducing the supersaturation that drives stone formation. Dietary modifications targeting sodium, animal protein, and oxalate intake may be recommended based on stone composition and metabolic findings. Thiazide diuretics, allopurinol, or citrate supplementation address specific metabolic abnormalities identified after ureteroscope treatment. This comprehensive approach extends the benefit of ureteroscope intervention beyond acute stone management to long-term prevention.
The ureteroscope has transformed the management of nephrolithiasis, providing a minimally invasive approach with excellent efficacy and favorable patient outcomes. Modern ureteroscope systems, particularly flexible digital instruments, allow access throughout the urinary tract with unprecedented visualization and therapeutic capabilities. Holmium:YAG laser lithotripsy through the ureteroscope effectively fragments stones of all compositions, while advanced retrieval devices facilitate fragment removal. The continued evolution of ureteroscope technology and techniques promises further improvements in stone-free rates and patient experience.
Successful ureteroscope management of nephrolithiasis requires more than technical proficiency with the instrument. Appropriate patient selection, thorough preoperative planning, attention to intraoperative details, and systematic postoperative care all contribute to optimal results. As ureteroscope technology advances and experience grows, the applications continue to expand, including complex stones and challenging anatomies. The ureteroscope remains a cornerstone of modern endourology, offering patients with nephrolithiasis a minimally invasive treatment option with demonstrated efficacy and safety.
The ureteroscope with holmium:YAG laser lithotripsy can effectively treat all stone compositions, including calcium oxalate, uric acid, struvite, and cysteine stones. The ureteroscope approach is particularly valuable for stones resistant to ESWL, such as cysteine and calcium oxalate monohydrate stones. The versatility of the ureteroscope across different stone types stems from the mechanism of holmium:YAG laser energy, which fragments stones through a photothermal process rather than mechanical means. This makes the ureteroscope an excellent choice regardless of stone composition when size and location are appropriate.
Recovery after ureteroscope procedures is typically rapid, with most patients resuming normal activities within 24-48 hours. Discomfort from the ureteroscope procedure itself usually resolves within a few days, though patients with ureteral stents may experience ongoing symptoms until stent removal. The minimally invasive nature of ureteroscope treatment contributes to this quick recovery, contrasting sharply with the prolonged convalescence after open stone surgery. Follow-up after ureteroscope procedures includes imaging to confirm stone-free status and may involve additional interventions for residual fragments.
The ureteroscope offers several advantages over alternative stone treatments, including high success rates, minimal invasiveness, and the ability to treat all stone types. Unlike ESWL, the ureteroscope provides direct visualization during treatment, confirming stone fragmentation and allowing retrieval of fragments. Compared to percutaneous nephrolithotomy, the ureteroscope approach involves no skin incision and decreased morbidity. The ureteroscope also enables treatment of stones throughout the entire urinary tract, from the distal ureter to the renal calyces, with a single instrument in many cases.
Stent placement after ureteroscope procedures is not always necessary, with increasing trends toward stentless ureteroscope approaches in selected patients. Factors favoring stent omission after ureteroscope procedures include minimal ureteral trauma, complete stone clearance, and absence of significant edema or obstruction. However, stents remain beneficial after ureteroscope procedures with prolonged operative time, significant ureteral manipulation, or concern about edema causing obstruction. The decision regarding stent placement after ureteroscope procedures individualizes based on intraoperative findings and patient factors.
Success rates for ureteroscope treatment of renal stones generally exceed 85-90% for stones less than 2cm, with experienced operators achieving even higher success rates. The ureteroscope consistently demonstrates excellent efficacy across various stone locations and compositions. Success depends on multiple factors, including stone burden, location, anatomy, and surgeon experience with ureteroscope techniques. For complex cases, staged ureteroscope procedures may be necessary to achieve complete clearance, particularly with large stone volumes. The high success rates of ureteroscope treatment have established it as a first-line option for many renal stones.
[1]https://uroweb.org/guideline/urolithiasis/
[2]https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4708572/
[3]https://www.sciencedirect.com
[4]https://onlinelibrary.wiley.com
[5]https://www.liebertpub.com