Views: 222 Author: Lake Publish Time: 2025-11-04 Origin: Site








Content Menu
>> Patient Evaluation and Consent
● Technique for Semirigid Ureteroscope Insertion
>> Cystoscopy and Ureteral Orifice Identification
>> Ureteroscope Insertion and Advancement
>> Stent Placement and Decision-Making
>> Equipment Processing and Maintenance
● Common Challenges and Solutions
>> 1. What is the optimal patient position for semirigid ureteroscopy in male patients?
>> 2. How can I manage difficulty in accessing the ureteral orifice?
>> 3. What are the indications for ureteral dilation before ureteroscope insertion?
>> 4. How high should the irrigation pressure be during ureteroscopy?
>> 5. When should a procedure be aborted due to access difficulties?
The semirigid ureteroscope has revolutionized modern urologic care, becoming an indispensable tool for diagnosing and treating various conditions within the upper urinary tract. As a minimally invasive instrument, the ureteroscope allows urologists to navigate the delicate urinary anatomy with precision, offering both diagnostic capabilities and therapeutic interventions. Since its introduction in the 1980s and the subsequent development of semi-rigid ureteroscope models in 1989, this technology has steadily evolved, providing improved flexibility without image distortion, making it the preferred choice for many urological procedures. For companies specializing in medical visualization devices, understanding the intricacies of ureteroscope insertion is crucial for developing products that meet the real-world demands of urologists and their patients.
The male urinary anatomy presents unique challenges for ureteroscope insertion, including a longer urethra, potential prostate enlargement, and naturally tortuous sections of the ureter. Mastering the technique of inserting a semirigid ureteroscope in male patients requires detailed knowledge of both the equipment and the anatomical considerations specific to male physiology. This article aims to provide a comprehensive, step-by-step guide to the proper insertion technique, drawing from current clinical practice and evidence-based approaches. We will explore preoperative preparation, detailed insertion methodology, postoperative care, and troubleshooting common challenges encountered during ureteroscope procedures.
As a company dedicated to advancing medical visualization technology, including ureteroscope systems, we recognize the importance of blending technical expertise with practical clinical application. The following sections will provide urologists and medical professionals with the essential knowledge to perform semi-rigid ureteroscopy safely and effectively in male patients, while also highlighting how our OEM services support the development of specialized ureteroscope equipment tailored to diverse clinical needs.

Successful ureteroscope insertion begins with thorough preoperative assessment. Each patient requires individual evaluation, including a detailed medical history focusing on prior urinary tract conditions, surgeries, or anatomical variations that might complicate the procedure. Specific attention should be paid to conditions such as prostate enlargement, urethral strictures, previous pelvic surgery or radiation, and any history of urinary tract reconstruction, as these factors significantly influence the approach to ureteroscope insertion.
Essential laboratory investigations include renal function tests and coagulation studies. Radiological assessment typically involves computed tomography (CT) scans or intravenous pyelography (IVP) to delineate the collecting system anatomy and identify any pathological obstructions. For stone procedures, a morning-of-surgery kidney, ureter, and bladder (KUB) X-ray or ultrasound may be useful to confirm the persistent presence of radiopaque stones, particularly at the ureterovesical junction (UVJ).
Informed consent is a critical component of the preoperative process. Patients should be thoroughly counseled about the risks associated with ureteroscope procedures, including the possibility of access failure, urinary tract trauma, postoperative infection, and the rare but serious risk of ureteral avulsion (less than 1%). Discussion should also cover the potential need for ureteral stent placement and the associated post-procedural symptoms.
Proper ureteroscope selection and preparation are fundamental to procedural success. The semirigid ureteroscope should be carefully inspected before each use to ensure optimal function. As part of the preparation process:
1. Ensure the ureteroscope is clean and sterile according to manufacturer guidelines.
2. Connect the ureteroscope to the camera adapter or use the eyepiece for direct visualization if not using camera systems.
3. Attach the light cable to the ureteroscope's light post.
4. Connect irrigation tubing to one of the working channels.
5. If using multiple instruments, attach the port seal valve to the other working channel (not used for irrigation) to maintain a closed system and prevent fluid leakage.
Additional essential equipment includes guidewires (both safety and working wires), which are crucial for maintaining access and minimizing trauma during repeated insertions of the ureteroscope. Guidewires typically feature flexible tips, low friction coatings (such as PTFE or hydrophilic polymers), and rigid shafts for better control. Other necessary instruments include stone extraction devices (often made of nitinol for their shape memory and kink resistance), intracorporeal lithotripters (pneumatic or laser, with Holmium:YAG laser being increasingly preferred), and ureteral stents of appropriate sizes.
Table: Essential Equipment for Semirigid Ureteroscopy
| Category | Specific Items | Purpose |
|---|---|---|
| Visualization | Semirigid ureteroscope, light source, camera system, irrigation fluid | Primary visualization and navigation |
| Access | Guidewires (safety and working), ureteral catheters | Establish and maintain ureteral access |
| Therapeutic | Stone baskets, forceps, lithotripsy devices | Treatment of pathologies |
| Safety | Stents, antibiotics, emergency equipment | Complication management and prevention |
Proper operating room configuration facilitates a smooth ureteroscope procedure. Male patients should be positioned in the dorsal lithotomy position, with adequate padding of all pressure points to prevent neurovascular injuries. This position provides optimal access to the urethral meatus and allows for natural anatomical alignment during ureteroscope insertion.
Anesthesia choice depends on patient factors and procedure complexity. While general anesthesia (GA) is often recommended for longer procedures due to better control of respiratory movements and the ability to temporarily halt ventilation if needed, spinal anesthesia or even intravenous sedation with local anesthesia may be appropriate for selected patients.
The equipment arrangement should prioritize ergonomics and efficiency. The C-arm for fluoroscopy and the endoscopy tower are ideally placed on the contralateral side to avoid interference between systems. Warm saline irrigation should be readily available and may be pressurized to ensure adequate visualization at the ureteroscope tip, though renal pelvic pressure should generally not exceed 30 cm H₂O to prevent postoperative pain, pyelorenal backflow, or fornix rupture. Radiation warning signs should be posted outside the operating room when fluoroscopy is in use.

The initial phase of ureteroscope insertion involves careful cystoscopic examination and identification of the ureteral orifice (UO). Before inserting the ureteroscope, perform a thorough cystoscopy to inspect the bladder and exclude any obvious pathology such as tumors or stones. During this examination:
- Maintain focus and white balance for optimal visualization.
- Avoid unnecessary trauma to the bladder neck, which is particularly important in males with prostatic enlargement.
- Systematically identify the bilateral ureteral orifices, which are typically located symmetrically along the interureteric ridge, 1-2 cm from the midline.
In male patients with benign prostatic hyperplasia (BPH) or median lobe enlargement, the ureteral orifices may be difficult to visualize due to obstruction or distortion of normal anatomy. If the UO is challenging to locate, try releasing bladder overdistension, as this may decompress the intramural ureters. Alternatively, withdraw the cystoscope to the bladder neck for better orientation of the interureteric ridge. The periodic ureteral peristalsis and efflux of urine from the orifice can also help in identification.
Once the ureteral orifice is identified, the next critical step is guidewire placement, which creates a safe pathway for ureteroscope advancement:
1. Position the cystoscope beak close to the UO, aligning it parallel to the orifice to facilitate safe guidewire insertion.
2. Gently advance the guidewire through the cystoscope working channel into the ureteral orifice.
3. If resistance is encountered, avoid applying excessive force, which may cause trauma or push stones backward.
4. For difficult cases, consider using a hydrophilic-tipped guidewire or a 5Fr open-ended ureteral catheter to navigate tortuous segments.
5. Fluoroscopic guidance can be helpful for visualizing wire progression, especially in cases with anatomical variations like fishhook (J-shaped) ureters, which are more common in males with prostate enlargement.
The European Association of Urology (EAU) guidelines recommend using a safety guidewire to allow for repeated non-traumatic access to the ureter and kidney. This safety wire should be securely placed in the renal pelvis before proceeding with ureteroscope insertion. An assistant may "fix" the wire to a stable sterile point to prevent dislodgement during the procedure.
With the safety guidewire securely in place, the semirigid ureteroscope can now be carefully inserted:
1. Urethral Insertion: Adequately lubricate the ureteroscope shaft before urethral insertion to reduce resistance. Hold the ureteroscope with your dominant hand while using the non-dominant hand to stabilize the instrument at the urethral meatus. Gently advance the ureteroscope through the urethra into the bladder under direct vision.
2. Approaching the Ureteral Orifice: Empty the bladder before attempting ureteral access to avoid compression of the intramural ureter and facilitate ureteroscope advancement. Position the ureteroscope near the UO, then advance it by "riding over" the guidewire or "creeping forward" under the wire. Use your left hand as a fulcrum to stabilize the ureteroscope during insertion.
3. Navigating the Intramural Ureter: This segment often presents the greatest resistance to ureteroscope advancement. Apply slight rotational movements—clockwise for the right ureter and counterclockwise for the left—to help the ureteroscope pass through the ureterovesical junction (UVJ). If resistance is significant, consider:
- Adding a second "railroad" wire to create a wider passage, with the ureteroscope advancing between the two wires.
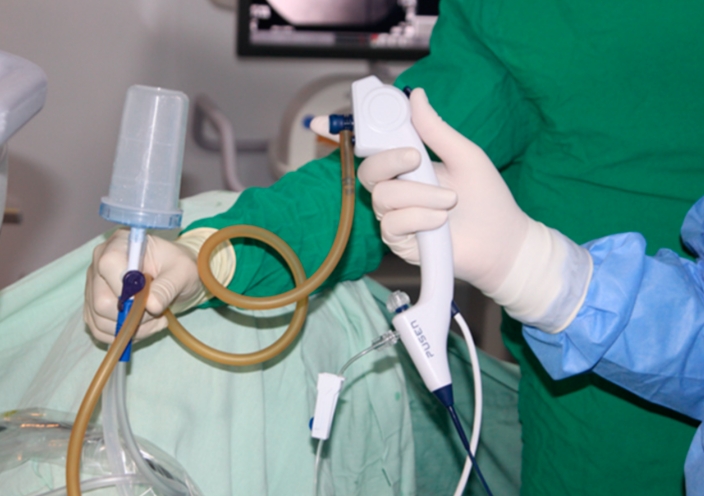
- Using pulsed irrigation with a 20mL syringe or a pressure-controlled irrigation system like the Uro-Pump to dilate the orifice.
- Employing sequential dilators or balloon dilators for stenotic segments.
4. Ascending the Ureter: Once past the UVJ, continue advancing the ureteroscope along the guidewire under direct vision. Maintain consistent irrigation through the ureteroscope working channel to distend the ureteral lumen and provide clear visualization. A Nelaton catheter placed in the urethra during the procedure provides continuous urinary drainage, helping to maintain low intrarenal pelvic pressure.
If you encounter mucosal folds or ureteral kinking during advancement, stop and wait for peristalsis to subside. For significantly kinked ureters, the double-wire technique can help straighten the path by creating a "railroad" track. If the ureteroscope cannot be advanced despite these maneuvers, avoid excessive force, which increases the risk of perforation. Instead, consider placing a ureteral stent for passive dilation and rescheduling the procedure for 7-14 days later.
The decision for postoperative ureteral stenting following ureteroscope procedures depends on several intraoperative factors. While routine pre-stenting is not necessary before ureteroscope intervention, postoperative stent placement is generally recommended in specific clinical scenarios. These include cases with documented ureteral trauma or perforation, impacted stones, solitary kidney, pregnancy, or history of retroperitoneal fibrosis.
Most urologists prefer maintaining ureteral stents for 1-2 weeks following ureteroscope procedures, though the ideal duration remains undefined. When placing a stent, keep the guidewire taut during insertion, and verify final position using both cystoscopy and fluoroscopy.
Stent-related symptoms are common in male patients and may include urinary frequency, urgency, dysuria, and pelvic discomfort. These can often be managed with medications such as alpha-blockers, anticholinergics, or analgesics. Proper patient counseling about expected stent symptoms and management options improves compliance and satisfaction.
Proper handling and maintenance of the semirigid ureteroscope are essential for instrument longevity and patient safety. After the procedure:
1. Cleaning: Rinse the ureteroscope under running potable water for at least one minute until it is no longer slippery. Flush the ureteroscope ports with water using a syringe. Inspect the ureteroscope for residual debris, particularly in hard-to-reach areas like the working channels. Repeat flushing if necessary until all debris is removed.
2. Drying: Wipe the ureteroscope with a soft, lint-free cloth until visible moisture is eliminated. Use compressed medical air to remove residual moisture from the channels.
3. Sterilization: Follow manufacturer instructions for sterilization, typically using glutaraldehyde solutions or other approved disinfectants. Do not reuse the instrument port seal valves, as they are designed for single use only.
To prevent damage to the semirigid ureteroscope, always handle it carefully—avoid dropping, impacting, cutting, or forcefully bending the outer sheath. When introducing instruments through the working channel, advance them slowly and gently. If any resistance is encountered, withdraw the instrument a few millimeters before continuing advancement.
Even with perfect technique, ureteroscope insertion in male patients can present unexpected challenges. Understanding these scenarios and their solutions enhances procedural success and patient safety:
1. Difficulty Identifying the Ureteral Orifice: In males with significant BPH, large median lobe, or distorted bladder anatomy, locating the ureteral orifice may be challenging. Techniques to improve identification include reducing bladder distention, using the guidewire to trace along the interureteric ridge, or intravenous injection of indigo carmine or methylene blue to visualize efflux. For tumors obscuring the orifice, transurethral resection with a bipolar loop may be necessary.
2. Ureteral Stenosis or Stricture: Narrowed ureteral segments may prevent ureteroscope advancement. If a smaller diameter ureteroscope cannot pass, consider balloon dilation or sequential plastic dilators. Balloon dilators appear safer than coaxial dilators, with fewer perforations. For refractory strictures, placement of a ureteral stent for passive dilation, followed by a delayed procedure 7-14 days later, is often effective.
3. Impacted Stones Obstructing Access: Stones lodged at the ureterovesical junction may prevent initial ureteroscope access. Techniques to manage this include using a grasper to extract the protruding stone, laser lithotripsy to fragment the obstruction, incising the stenotic ureteral orifice, or using a Collins loop to dislodge the stone.
4. Guidewire Resistance or Perforation: If the guidewire meets resistance during initial placement, avoid excessive force. Instead, try using a hydrophilic guidewire, which can often navigate around obstructions with lower false passage risk. If guidewire integrity is compromised during the procedure, gently apply steady traction to remove it and inspect the tip for damage.
5. Significant Ureteral Tortuosity: In cases of pronounced ureteral kinking, especially in the proximal ureter, the double-wire technique can help straighten the path. Alternatively, using a ureteral access sheath may provide more stable access for flexible ureteroscope procedures, though this is more commonly used in conjunction with flexible rather than semirigid ureteroscopes.
For cases where ureteroscope access remains impossible despite these techniques, aborting the procedure and placing a stent for passive dilation followed by a second attempt after 1-2 weeks is the safest approach. Recognizing when to stop attempting access is as important as mastering advancement techniques, as persistence in the face of significant resistance may lead to severe ureteral damage.
The successful insertion of a semirigid ureteroscope in male patients requires a systematic approach that blends anatomical knowledge, technical skill, and appropriate technology. From thorough preoperative planning to meticulous technique and postoperative care, each step contributes to the procedure's overall success and safety. The male urinary tract, with its longer urethra and potential anatomical challenges like prostate enlargement, demands particular attention to detail during ureteroscope advancement. Mastering the techniques of guidewire placement, ureteral orifice navigation, and troubleshooting common obstacles enables urologists to maximize the therapeutic potential of ureteroscope procedures while minimizing complications.
Advances in ureteroscope technology continue to expand the boundaries of minimally invasive urology. As manufacturers develop slimmer profiles, improved optics, and enhanced flexibility in semirigid ureteroscope designs, the procedures become accessible to more patients with complex anatomy. For companies operating in the medical visualization space, understanding these clinical nuances informs the development of next-generation ureteroscope systems that offer improved performance and patient outcomes. Through continued collaboration between clinicians and manufacturers, the field of endourology will continue to evolve, maintaining ureteroscopy as a cornerstone of modern urologic practice.
Male patients should be positioned in the dorsal lithotomy position with adequate padding of all pressure points to prevent neurovascular injuries. This position provides optimal access to the urethral meatus and aligns the urethral and ureteral anatomy to facilitate ureteroscope insertion. Ensure the position is comfortable and sustainable, as prolonged procedures may require repositioning to prevent complications.
If the ureteral orifice is difficult to access, try reducing bladder distention to decompress the intramural ureters. Other techniques include using the guidewire to trace along the interureteric ridge, looking for urine efflux, or using intravenous indigo carmine or methylene blue to visualize the orifice. For cases with significant anatomical obstacles, using the ureteroscope itself under direct vision to insert the guidewire may be helpful.
Ureteral dilation may be necessary when the ureteroscope cannot pass through a narrow segment despite appropriate techniques. This can be achieved actively using balloon dilators or sequential plastic dilators, or passively by placing a stent and delaying the procedure for 7-14 days. Balloon dilators appear safer than coaxial dilators, with fewer associated perforations.
Irrigation pressure should be sufficient to maintain clear visualization but generally should not exceed 30 cm H₂O in the renal system to prevent postoperative pain, pyelorenal backflow, or fornix rupture. Pressure-controlled irrigation systems like the Uro-Pump can optimize intraoperative pressure control while maintaining an excellent visual field.
If the ureteroscope cannot be advanced despite using techniques like guidewire placement, rotation, irrigation, or dilation, and significant resistance remains, it is safer to abort the procedure and place a stent for passive dilation. A second attempt after 7-14 days often proves successful once the ureter has been passively dilated. Forcing the ureteroscope against resistance significantly increases the risk of ureteral perforation or avulsion.