Views: 222 Author: Lake Publish Time: 2025-12-27 Origin: Site








Content Menu
● Understanding the Laryngoscope Handle: Types and Risks
● General Principles and Pre-Cleaning
● Step-by-Step Cleaning and Disinfection for Reusable Metal Handles
>> Phase 1: Manual Cleaning (The Most Critical Step)
>> Phase 2: Disinfection or Sterilization
>> Phase 3: Drying, Reassembly, and Storage
● Special Considerations for Video Laryngoscope Handles
● Common Errors and How to Avoid Them
● The Role of Single-Use Covers and Disposable Options
● Frequently Asked Questions (FAQ)
>> 1. Can I clean a laryngoscope handle by simply wiping it with an alcohol swab?
>> 2. How often should the batteries in a reusable laryngoscope handle be changed?
>> 3. Is it acceptable to store the laryngoscope handle with the blade attached?
>> 4. What should I do if a laryngoscope handle is damaged (cracked, corroded, broken latch)?
>> 5. What is the advantage of using a disposable plastic sheath over a laryngoscope handle?
In the critical practice of airway management, the laryngoscope is an indispensable tool. While much focus is rightly placed on the cleaning and disinfection of the blade—the part that enters the patient's airway—the laryngoscope handle demands equally rigorous attention. The handle, frequently touched by clinicians' hands, can become a reservoir for pathogens, posing a significant risk of cross-contamination. Proper cleaning and disinfection of the laryngoscope handle are therefore fundamental components of infection prevention and control protocols. This comprehensive guide details the correct procedures for cleaning, disinfecting, and maintaining laryngoscope handles, covering both reusable and disposable types, and emphasizes the importance of adhering to manufacturer instructions and institutional policies to ensure patient safety and device longevity.
As a company involved in the OEM manufacturing of medical visualization devices, we understand that the durability and cleanability of a laryngoscope handle are key design considerations. The following protocols align with the standards expected of high-quality medical equipment.

Before cleaning, it's essential to identify the type of laryngoscope handle, as this determines the appropriate reprocessing method.
1. Reusable Metal Handles: The traditional and most common type, typically made of stainless steel or chrome-plated brass. They are durable, designed for repeated use, and must undergo reprocessing between each patient use. They house the batteries that power the light source.
2. Disposable Handles: Made of plastic, these are for single use and are discarded after a procedure. They are often pre-assembled with a blade. While they eliminate reprocessing, they still require proper disposal as medical waste.
3. Rechargeable/Dedicated System Handles: Used with video laryngoscope systems or specific proprietary brands. These often have electronic components, screens, or charging ports and require very specific cleaning procedures to avoid liquid ingress.
The laryngoscope handle is considered a semi-critical item (contacting mucous membranes or non-intact skin). According to Spaulding's Classification, it requires at least high-level disinfection (HLD), though sterilization is preferred when possible. However, its construction often limits it to HLD or low-level disinfection of external surfaces, depending on design.
Universal Precautions: Always treat every laryngoscope handle as potentially contaminated. Wear appropriate personal protective equipment (PPE)—gloves and a gown—during cleaning.
Point-of-Care Wipe Down: Immediately after use, before transferring to the reprocessing area, wipe the laryngoscope handle with a cloth dampened with a hospital-grade disinfectant. This removes gross contamination and reduces bioburden.
Consult the Manufacturer's Instructions for Use (IFU): This is the most critical step. The IFU provides the only approved methods for cleaning and disinfection that will not void warranties or damage the device. The following steps are a general framework but must be validated against the specific IFU.
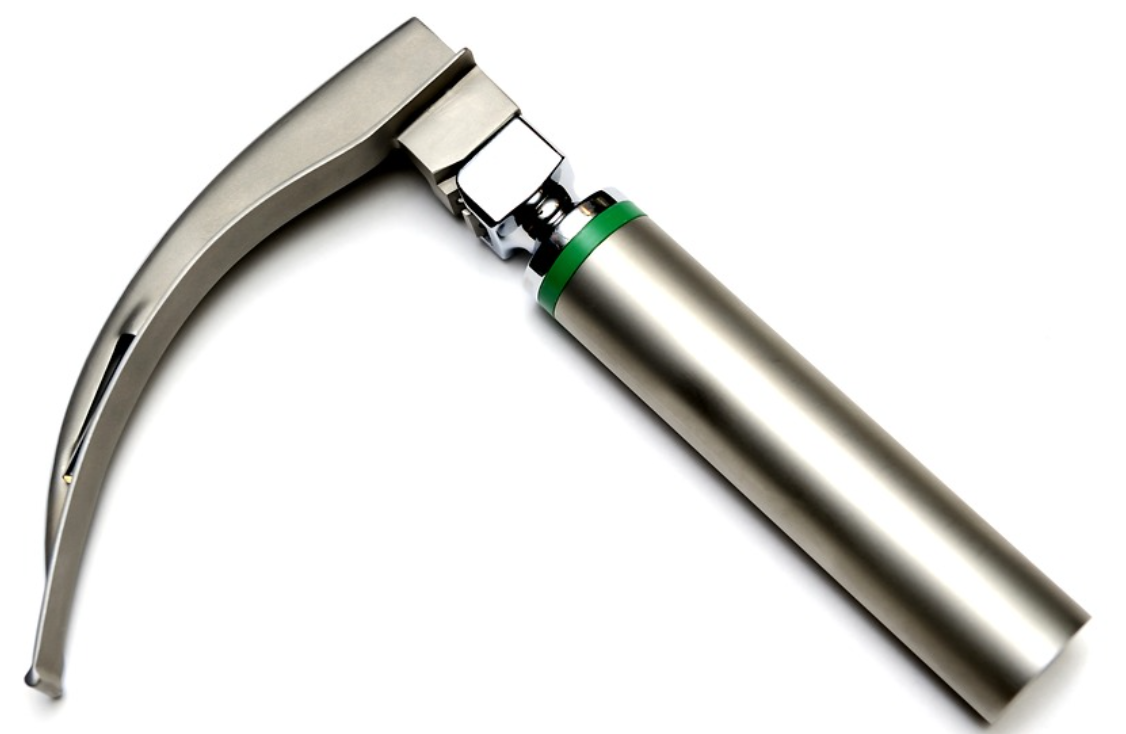
Effective disinfection is impossible without prior thorough cleaning to remove organic material (blood, saliva).
1. Disassembly: Remove the laryngoscope blade. For handles with a removable bulb housing or bottom cap, open these according to the IFU to access the battery compartment.
2. Battery Removal: Always remove the batteries. Cleaning a laryngoscope handle with batteries inside can lead to corrosion, electrical failure, and inadequate disinfection of internal contacts.
3. Pre-Rinse: Rinse the handle under lukewarm running water to remove loose debris.
4. Washing:
- Prepare a basin with warm water and a compatible, neutral pH enzymatic detergent.
- Using a soft, lint-free cloth or a soft-bristled brush dedicated to medical instrument cleaning, thoroughly wash all external surfaces of the laryngoscope handle. Pay special attention to crevices, the blade locking mechanism, and any textured grip areas.
- If the IFU permits immersion, submerge the handle and gently agitate. Never immerse a handle unless the IFU explicitly states it is immersible.
5. Internal Contact Cleaning: Using a cotton swab or small brush moistened with detergent, gently clean the battery compartment interior and the electrical contacts.
6. Rinsing: Thoroughly rinse the laryngoscope handle under clean, running water to remove all detergent residue. Residue can inactivate disinfectants.
A. High-Level Disinfection (HLD): This is the standard for most reusable laryngoscope handles.
- Chemical Disinfection: If the IFU allows, immerse the handle in an EPA-registered hospital-grade disinfectant (e.g., glutaraldehyde, ortho-phthalaldehyde, peracetic acid) for the exact contact time specified by the disinfectant manufacturer and the laryngoscope IFU.
- Wipe Disinfection: If immersion is not permitted (common for most standard handles due to battery contact risks), use a cloth saturated with the disinfectant to thoroughly wet all surfaces of the laryngoscope handle and maintain wet contact for the required time (e.g., 3-10 minutes, depending on the agent).
B. Sterilization: Preferred but not always possible.
- Low-Temperature Sterilization: Some laryngoscope handles are compatible with hydrogen peroxide gas plasma (e.g., Sterrad) or ethylene oxide (EtO) sterilization. This is ideal but requires specific packaging and cycle time.
- Autoclaving (Steam Sterilization): Most standard laryngoscope handles with plastic components, seals, or electronics are NOT autoclavable. Autoclaving will destroy them. Only handles specifically labeled as "autoclavable" can undergo this process.
1. Drying: After disinfection, air-dry the laryngoscope handle completely on a clean, lint-free towel in a low-dust environment. Use a compressed air duster to remove moisture from the battery compartment and contacts if needed. Ensure it is bone dry before inserting batteries to prevent corrosion.
2. Inspection and Functional Check: Visually inspect for damage or residual soil. Insert fresh batteries and attach a clean blade to check the light function. A bright, steady light confirms electrical integrity.
3. Storage: Store the fully assembled, tested laryngoscope in a clean, dry, protected storage cabinet or drawer. It should be ready for immediate use.
Handles for video laryngoscope systems are more complex and require extra care.
1. Strict Adherence to IFU: Their reprocessing is highly specific. Never assume immersion is allowed.
2. Wipe-Down Only: Most require careful, meticulous wiping with approved disinfectant wipes. Avoid getting moisture into ports, vents, or screen edges.
3. Separate Components: Often, the video blade (containing the camera) is detached and reprocessed separately (sometimes in an AER). The handle, containing electronics and a screen, is only wiped.
4. Battery Management: Follow instructions for charging and battery removal/replacement during cleaning.
- Not Removing Batteries: This is the most common error, leading to corrosion and device failure.
- Using Abrasive Materials: Steel wool or harsh scrubbing pads can scratch the laryngoscope handle's finish, creating niches where bacteria can hide.
- Incomplete Drying: Storing a damp handle promotes microbial growth and battery corrosion.
- Using Incompatible Chemicals: Alcohol can damage rubber seals and plastic. Bleach can corrode metal. Always use manufacturer-approved agents.
- Neglecting the Battery Compartment: This area is a critical hidden surface that must be cleaned.
To simplify the process and guarantee infection control, many institutions use:
- Disposable Laryngoscope Blade and Handle Systems: Entirely single-use, eliminating reprocessing.
- Clear Plastic Sheath/Covers: A sterile, disposable plastic sleeve is placed over a cleaned laryngoscope handle before each use. This provides a barrier, meaning only the sheath contacts the patient/operator, and the handle requires only low-level disinfection between patients. The sheath must be changed between every patient.
Cleaning a laryngoscope handle is a non-negotiable, proceduralized task that sits at the intersection of clinical efficacy and patient safety. It is a multi-step process that begins with immediate point-of-care decontamination and proceeds through meticulous manual cleaning, appropriate disinfection (or sterilization where possible), and thorough drying and testing. The cornerstone of this process is unwavering adherence to the device-specific Manufacturer's Instructions for Use.
Given the complexities and risks, the trend towards single-use laryngoscope systems or the use of disposable handle sheaths presents a compelling solution, effectively outsourcing the reprocessing burden to the manufacturer and providing the highest assurance against cross-contamination. Whether maintaining reusable equipment or utilizing disposable barriers, a rigorous, consistent protocol for laryngoscope handle hygiene is an essential investment in preventing healthcare-associated infections and ensuring that this vital airway tool is always safe and ready for its next life-saving use.

No, alcohol swabs are insufficient for proper disinfection of a laryngoscope handle. While alcohol is effective against many pathogens, it is not a high-level disinfectant for all viruses and spores. More importantly, alcohol can degrade rubber seals and plastic components over time. You must use an EPA-registered hospital-grade disinfectant wipe or solution approved by the laryngoscope manufacturer.
Batteries should be changed before every use or at the start of each clinical shift. A functional check with a new blade should always be performed. Never use a laryngoscope with weak or old batteries, as a dim light compromises visualization and patient safety. Remove batteries for storage to prevent leakage and corrosion.
It is generally recommended to store them separately. Storing with the blade attached can place stress on the locking mechanism and potentially dull the blade. Furthermore, separate storage in a clean, organized tray or cabinet allows for easy visual inspection and access. The handle should be fully assembled (with batteries and a clean blade) only when prepared for immediate use in a procedure.
Immediately remove it from clinical service. A damaged laryngoscope handle is a patient and staff safety hazard. It can fail during intubation, harbor pathogens in cracks, or have electrical faults. Tag it clearly as "DEFECTIVE" and follow your facility's protocol for medical device repair or disposal. Do not attempt to use it.
The primary advantage is simplified infection control and workflow efficiency. The sterile sheath creates a physical barrier. After use, only the sheath is contaminated and is discarded. The underlying laryngoscope handle requires only a low-level wipe down between patients, not full high-level disinfection. This reduces reprocessing time, eliminates risks associated with incomplete cleaning, and extends the functional life of the handle by minimizing exposure to harsh chemicals.
[1] https://www.cdc.gov/infectioncontrol/guidelines/disinfection/index.html
[2] https://www.fda.gov/medical-devices/reprocessing-reusable-medical-devices
[3] https://www.apsf.org/article/guidelines-for-laryngoscope-handle-cleaning/
[4] https://www.asahq.org/standards-and-guidelines/guidelines-for-cleaning-and-processing-anesthesia-equipment
[5] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2866602/
[6] https://www.rcoa.ac.uk/safety-standards-quality/guidance-resources/guidelines-cleaning-laryngoscopes
[7] https://www.astm.org/Standards/medical-devices-standards.html