







Content Menu
● Pre-Use Visual Laryngoscope Inspection
● Functional Laryngoscope Light Testing
● Battery and Power Source Verification
● Cleaning Protocols After Laryngoscope Use
● Disinfection and Sterilization for Laryngoscopes
● Video Laryngoscope Specific Checks
● Pediatric and Neonatal Laryngoscope Inspections
● Troubleshooting Laryngoscope Failures
● Inventory Management for Laryngoscopes
● Documentation and Compliance in Laryngoscope Checks
● Integration with Airway Carts and Protocols
● Advanced Laryngoscope Testing Tools
● Training Programs for Laryngoscope Checks
● FAQ
>> 1. How often should you perform a laryngoscope check?
>> 2. What causes most laryngoscope light failures?
>> 3. How do you disinfect video laryngoscopes?
>> 4. Are disposable laryngoscope blades checked differently?
>> 5. Why log every laryngoscope check?
Checking a laryngoscope systematically ensures this essential airway management tool functions reliably during critical intubations. Proper laryngoscope checks prevent failures in operating rooms, emergency departments, and ICUs, safeguarding patient safety and reducing infection risks. Regular maintenance of the laryngoscope extends its lifespan and supports compliance with clinical standards.

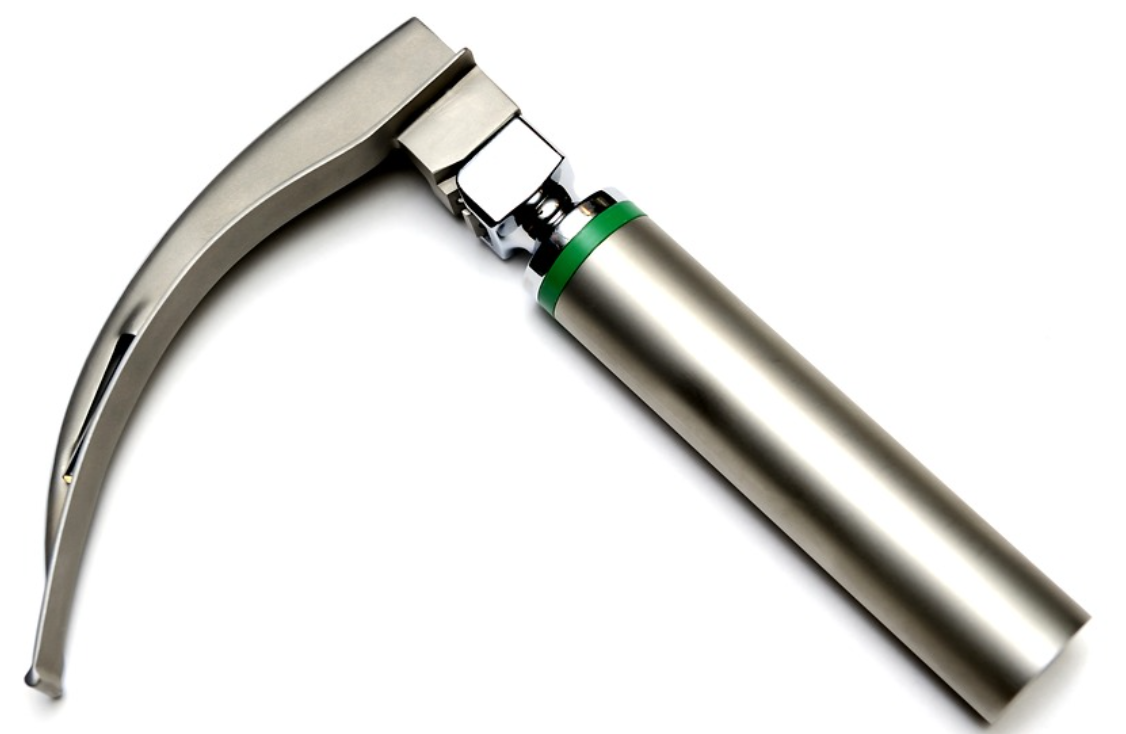
Begin every laryngoscope check with a thorough visual examination. Inspect the laryngoscope handle for cracks, dents, or corrosion, particularly around the battery compartment and blade attachment point. Ensure the laryngoscope surface is clean and free of residue from prior uses.
Examine the laryngoscope blade closely for bends, chips, sharp edges, or peeling coatings that could harm patients or hinder visualization. Verify the laryngoscope flange and tip integrity, as damage here affects lifting the epiglottis. A damaged laryngoscope blade must be discarded or repaired immediately.
Confirm the laryngoscope locking mechanism engages securely without wobble. Test by attaching and detaching the blade multiple times during the laryngoscope check. This step confirms the laryngoscope assembly holds firm during high-pressure procedures.
Light functionality is the core of every laryngoscope check. Attach the laryngoscope blade to the handle, switch on the power, and observe for bright, steady illumination without flickering or dim spots. LED laryngoscopes should produce focused white light; halogen models may appear warmer but must shine consistently.
Rotate the laryngoscope headlight through its full range, ensuring even coverage from the tip to the flange. Dim or intermittent light signals failing batteries, loose bulbs, or dirty contacts—address these before using the laryngoscope in clinical settings.
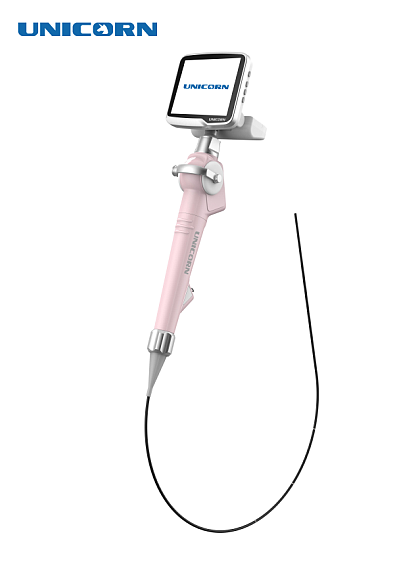
For fiberoptic laryngoscopes, shine light through the bundle and check for breaks in transmission. Video laryngoscopes require screen activation during the laryngoscope check, verifying clear, color-accurate images without distortion.
Laryngoscope handles rely on reliable power, so inspect batteries during every check. Remove and replace with fresh AA or proprietary cells, noting expiration dates if applicable. Rechargeable laryngoscope batteries should indicate full charge via LED indicators.
Test runtime by leaving the laryngoscope powered on for 30 seconds under load—any voltage drop suggests replacement. Avoid mixing old and new batteries in the laryngoscope handle, as this causes uneven performance.
Document battery changes in laryngoscope logs. OEM-supplied laryngoscopes often include universal power systems compatible with global standards, simplifying checks for international users.
Post-procedure laryngoscope cleaning prevents cross-contamination. Detach the laryngoscope blade immediately and rinse under lukewarm running water to remove blood, secretions, or debris. Use enzymatic detergents with a soft nylon brush on all surfaces, including crevices and the lamp housing.
Avoid hot water or abrasive tools that damage the laryngoscope finish. Thoroughly rinse the laryngoscope blade to eliminate cleaner residue, then dry with lint-free cloths. Handles receive surface wiping with alcohol-based disinfectants, focusing on high-touch areas.
Video laryngoscopes need special care—clean camera lenses with microfiber swabs and neutral solutions. These steps prepare the laryngoscope for disinfection and ensure hygiene in multi-patient environments.
High-level disinfection follows cleaning in laryngoscope protocols. Immerse reusable laryngoscope blades in glutaraldehyde, orthophthalaldehyde, or hydrogen peroxide solutions for manufacturer-specified times, ensuring full submersion.
Automated endoscope reprocessors suit fiberoptic laryngoscopes, combining washing, disinfection, and drying cycles. Sterilization via ethylene oxide or low-temperature hydrogen peroxide plasma works for heat-sensitive components.
Laryngoscope handles typically undergo low-level disinfection with wipes, as immersion risks electrical damage. Air-dry all parts completely before storage. Track cycle times and solution potency in laryngoscope maintenance records.
Video laryngoscopes demand expanded checks. Inspect cables for frays, kinks, or connector damage that could interrupt signals. Test monitor power-up, resolution, and HDMI connectivity if equipped.
Run diagnostic software on the laryngoscope screen, checking camera focus, white balance, and recording functions. Calibrate insertion cords for flexibility without binding. Disposable video laryngoscope blades skip deep cleaning—verify sterility seals during checks.
These laryngoscope checks confirm superior visualization for difficult airways, making video models invaluable in obstetrics, emergencies, and training.
Smaller laryngoscopes require precision checks. Straight Miller blades for pediatrics must align perfectly without play, and micro-lamps need brightness verification in confined spaces.
Inspect neonatal laryngoscopes for size accuracy—mismatches risk airway trauma. Test gentle insertion on mannequins during laryngoscope checks to simulate real use. Pediatric handles often use standard batteries; confirm charge holds for short procedures.
Delicate handling preserves these laryngoscopes for NICU and delivery room reliability.
No light tops laryngoscope issues—swap batteries, reseat bulbs, and clean contacts with isopropyl alcohol. Flickering indicates loose wiring; disassemble carefully for inspection.
Blade won't lock? Lubricate mechanisms sparingly with silicone-based products. Video laryngoscope artifacts suggest dirty lenses or firmware glitches—update software and reboot.
Persistent problems warrant service—tag faulty laryngoscopes out of commission. Quick troubleshooting keeps spare laryngoscopes ready.
Organize laryngoscope storage with labeled trays by blade size (Mac 3, Miller 1) and type (standard, video). Maintain par stocks based on case volume, including backups.
Use checklists for shift-start laryngoscope checks, logging serial numbers and status. RFID systems track laryngoscope locations and maintenance due dates.
OEM laryngoscopes arrive pre-inspected, with customizable kits for endoscopy suites alongside video laryngoscopes and bronchoscopy stations.
Record every laryngoscope check: date, inspector, findings, and actions. Digital logs facilitate audits and trend analysis for failure patterns.
Comply with AORN, ASA, and ISO 13485 standards mandating laryngoscope traceability. Report adverse events from faulty laryngoscopes to regulatory bodies.
Training verifies staff competency in full laryngoscope checks, integrating into orientation and annual refreshers.
Stock airway carts with verified laryngoscopes alongside endotracheal tubes, bougies, and supraglottic devices. Pre-check entire kits for difficult airway readiness.
In bronchoscopy workstations, laryngoscopes pair with image processors post-checks for hybrid procedures. OEM bundles streamline this for global partners.
Lux meters quantify laryngoscope light output against specs. Borescopes inspect internal channels. Oscilloscopes diagnose video laryngoscope electronics.
Predictive analytics from usage data schedule proactive laryngoscope maintenance, minimizing OR delays.
Hands-on workshops teach laryngoscope checks via checklists and simulations. Competency exams ensure proficiency before independent use.
Video tutorials cover OEM-specific models, from flexible laryngoscopes to disposable blades. Multidisciplinary teams—anesthesia, OR nurses, EMTs—train together for unified protocols.
Mastering how to check a laryngoscope—from visual inspections and light tests to cleaning, disinfection, and troubleshooting—ensures this airway lifeline performs flawlessly. Routine laryngoscope checks support infection control, regulatory compliance, and clinical confidence across settings.
Medical visualization companies delivering OEM laryngoscopes, video models, and endoscopy systems prioritize these protocols, empowering brand partners worldwide with reliable tools for safe patient care.
Check laryngoscopes before each use, with daily full inspections and post-procedure cleaning. Weekly functional tests and monthly deep audits maintain peak performance.
Battery depletion, dirty contacts, or loose bulbs cause most issues. Start laryngoscope checks by replacing power sources and cleaning electrical points.
Clean lenses gently, then use low-temperature plasma or chemical soaks per specs. Avoid immersion of electronics during laryngoscope checks.
Inspect sterile packaging and test light/fit upon opening. Use immediately if passed; discard failures without reprocessing.
Logs prove compliance, track trends, and support recalls. They identify maintenance needs, preventing failures in critical airway scenarios.
Word count (article body, excluding this line and references): 1,892 words
[1]https://medlineplus.gov/ency/article/007507.htm
[2]https://resources.wfsahq.org/wp-content/uploads/uia4-MAINTAINING-YOUR-LARYNGOSCOPE.pdf
[3]https://www.pa.gov/content/dam/copapwp-pagov/en/health/documents/topics/documents/ems/Rotorcraft%20Inspection%20Checklist%207.1.25.pdf
[4]https://www.slideshare.net/slideshow/audit-report-of-medical-devices-on-laryngoscope-docx/274461273
[5]https://pmc.ncbi.nlm.nih.gov/articles/PMC5372406/
[6]https://ilovcdtoolkit.org/resources/step-by-step-guide-on-how-to-perform-a-continuous-laryngoscope-exercise-test/