Views: 222 Author: Lake Publish Time: 2026-01-18 Origin: Site








Content Menu
● Introduction: Defining the Instruments and Anatomy
● The Role of the Laryngoscope in Head and Neck Examination
● The Correct Tool: Nasal Endoscopy (Rhinoscopy)
● The Definitive Visualization: Endoscopic Sinus Surgery (ESS)
● The Comprehensive Diagnostic Pathway for Suspected Sinus Cancer
● The Evolving Role of Advanced Visualization
● Frequently Asked Questions (FAQ)
>> 1. What is the main difference between a laryngoscope and a nasal endoscope?
>> 2. What procedure would a doctor use to actually look inside my sinuses?
>> 4. What are the typical symptoms that might lead to an endoscopic examination for sinus cancer?
>> 5. Can newer video laryngoscopes with cameras see more than older models?
In the precise and evolving field of otolaryngology and head and neck oncology, the accurate diagnosis of pathology depends on matching the appropriate visualization tool to the anatomical region of interest. A common diagnostic question arises: can a laryngoscope be used to detect sinus cancer? This article provides a definitive, anatomically grounded explanation, detailing the scope and limitations of the laryngoscope, introducing the correct endoscopic tools for sinus evaluation, and outlining the comprehensive diagnostic pathway for suspected sinus malignancies.
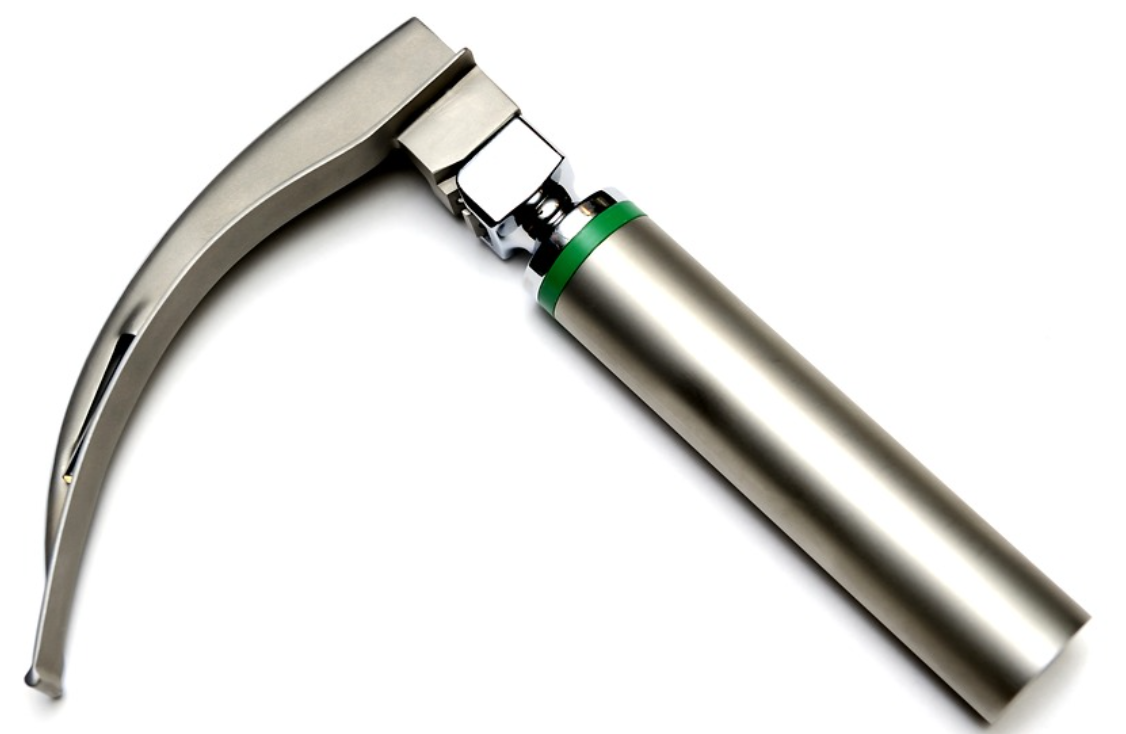
To answer this question, one must clearly understand what a laryngoscope is designed to visualize. A laryngoscope is an instrument specifically intended for examining the larynx (voice box). It provides a view of the structures from the base of the tongue down to the vocal cords and the upper trachea. The paranasal sinuses (maxillary, ethmoid, frontal, and sphenoid), however, are air-filled cavities located within the bones of the face and skull, above the palate and around the nasal cavity. They have no direct anatomical connection to the larynx that is accessible by the standard path of a laryngoscope.
Therefore, the direct and short answer is: No, a standard laryngoscope cannot visualize the interior of the paranasal sinuses where sinus cancer typically originates.
While it cannot see into the sinuses, a laryngoscope—particularly a flexible laryngoscope or video laryngoscope—plays a crucial indirect and evaluative role in the context of sinonasal cancer:
1. Assessment of Secondary Extension: Advanced sinus cancers, especially those originating in the maxillary or ethmoid sinuses, can grow inferiorly to invade the hard palate, the nasopharynx, or even extend into the oropharynx. A flexible laryngoscope passed through the nose can assess the nasopharynx (the space behind the nose) for bulging or obstruction from a superior tumor. It can also be used to examine the oropharynx and hypopharynx for any downward spread.
2. Evaluation of Vocal Cord Function: Sinus cancers that affect the skull base may involve the nerves that control the vocal cords (e.g., the vagus nerve or its recurrent laryngeal branch). A laryngoscope is the essential tool for assessing vocal cord mobility, and paralysis can be a critical sign of advanced disease.
3. Rule-Out of Synchronous Primaries: Patients with head and neck cancer have a higher risk of a second, separate cancer in the aerodigestive tract. A complete examination with a laryngoscope is standard to inspect the larynx and pharynx for any other lesions.
The primary endoscopic tool for evaluating the sinuses is a nasal endoscope (or rhinoscope). This is a type of endoscope system, but it is distinct from a laryngoscope.
- Design: Nasal endoscopes are typically rigid, rod-lens telescopes with varying angles of view (0°, 30°, 70°). They are shorter and often have a different diameter and optics optimized for the nasal cavity.
- Procedure (Nasal Endoscopy): The endoscope is gently passed along the floor of the nasal cavity under local anesthesia. It allows direct visualization of:
- The nasal mucosa, septum, and turbinates.
- The ostiomeatal complex – the critical drainage pathways for the maxillary, frontal, and anterior ethmoid sinuses.
- The sphenoethmoidal recess and the opening of the sphenoid sinus.
- The nasopharynx and the orifice of the Eustachian tube.
- What Can Be Seen: An experienced otolaryngologist can identify indirect signs of sinus pathology such as:
- Purulent drainage from a sinus ostium.
- Polypoid tissue or mass protruding from a sinus opening.
- Bulging of the medial wall of the maxillary sinus (the lateral nasal wall).
- Areas of abnormal bleeding or necrotic tissue.
While a nasal endoscope cannot see inside a healthy sinus cavity, it can reveal the drainage pathways and detect masses that extend into or obstruct the nasal cavity.

To directly visualize the interior of a sinus where cancer is suspected, a procedure called endoscopic sinus surgery (ESS) is required. This is performed in an operating room under general anesthesia.
- Technology: Surgeons use the same or similar rigid nasal endoscopes, often connected to a high-definition medical image processor and display, similar to a bronchoscopy workstation setup.
- Procedure: Using specialized instruments, the surgeon can carefully open (widen) the natural sinus ostium or create a controlled portal to access the sinus cavity directly. This allows for:
- Direct inspection of the sinus mucosa.
- Biopsy of suspicious tissue for definitive histopathological diagnosis.
- Assessment of tumor extent within the sinus and its relationship to critical structures like the orbit, skull base, and major blood vessels.
Diagnosis relies on a multi-modal approach, where endoscopy is one key component:
1. Clinical History and Examination: Symptoms like unilateral nasal obstruction, bloody discharge, facial pain or numbness, and eye symptoms (proptosis, diplopia) raise suspicion.
2. Nasal Endoscopy: The first-line endoscopic procedure to look for intranasal masses, polyps, or discharge.
3. Cross-Sectional Imaging (CT and MRI): This is the cornerstone for evaluating sinus cancer. A CT scan details bony erosion, while an MRI excels at defining soft tissue extent, perineural spread, and intracranial or orbital invasion. Imaging guides the endoscopic biopsy.
4. Endoscopic Biopsy (in-clinic or during ESS): Tissue sampling under endoscopic visualization provides the pathological diagnosis.
5. Panendoscopy: This is a comprehensive endoscopic examination under anesthesia, which may include laryngoscopy, pharyngoscopy, esophagoscopy, and bronchoscopy. This is performed to stage the primary tumor fully and to rule out synchronous cancers elsewhere in the upper aerodigestive tract. Here, a laryngoscope is used as part of a broader survey.
Technology is enhancing diagnosis:
- High-Definition and 4K Video Endoscopes: Provide exceptional image clarity for detecting subtle mucosal changes.
- Narrow Band Imaging (NBI): An optical filter technology available on some endoscope systems that enhances the visualization of submucosal blood vessels, potentially helping to distinguish benign from malignant tissue.
- Integrated Imaging: Systems that allow navigation using pre-operative CT scans during ESS, providing real-time guidance for biopsy and tumor mapping.
A laryngoscope is an invaluable tool for examining the larynx and lower pharynx, but its anatomical reach does not extend to the paranasal sinuses. Therefore, it cannot directly visualize sinus cancer. Suspicion of sinus malignancy begins with a thorough nasal endoscopy to assess the nasal cavity and sinus drainage pathways, followed indispensably by cross-sectional CT and MRI imaging. Direct visualization and biopsy of a sinus tumor typically require endoscopic sinus surgery. In the comprehensive workup, a laryngoscope plays a vital secondary role in assessing for tumor extension, nerve involvement affecting the voice, and screening for secondary cancers. This delineation of instrument purpose underscores a fundamental principle in medical visualization: choosing the right tool for the right anatomy is the first step toward accurate diagnosis and effective treatment planning, a principle that guides our own development of specialized devices from disposable ureteroscopes to video laryngoscopes.
Contact us to get more information!

The primary difference is anatomical target and design. A laryngoscope (flexible or rigid) is designed to visualize the larynx (voice box) and is typically inserted through the mouth or sometimes the nose to look downwards. A nasal endoscope (usually rigid) is designed to visualize the nasal cavity and sinus drainage pathways and is inserted through the nostril to look upwards and laterally into the nasal architecture. They are different tools within the broader family of endoscope systems.
To directly visualize the interior of your sinuses, a doctor would perform Endoscopic Sinus Surgery (ESS). This is a surgical procedure done under general anesthesia. Using thin, rigid nasal endoscopes connected to a camera and monitor, the surgeon can gently open the natural sinus openings to access and inspect the sinus cavities, take biopsies, or remove tissue. An in-office nasal endoscopy can only see the openings of the sinuses, not inside them.
An ENT may use a flexible laryngoscope during a sinus evaluation for several important reasons:
1. To examine the nasopharynx (the space behind the nose) for any extension of a sinus tumor.
2. To check vocal cord function, as some advanced sinus cancers can affect the nerves controlling the voice.
3. To perform a complete survey of the upper airway to rule out other unrelated issues or secondary tumors, which is a standard part of a comprehensive head and neck exam.
Symptoms that warrant endoscopic evaluation include:
- Persistent, one-sided nasal obstruction or congestion.
- Facial pain, pressure, or numbness (especially in the cheek or upper teeth).
- Persistent one-sided nosebleeds (epistaxis).
- Bloody nasal discharge.
- Reduced sense of smell.
- Eye symptoms such as bulging, double vision, or pain.
- A palatal mass or loosening of upper teeth.
Modern video laryngoscopes offer superior image resolution, magnification, and the ability to record findings. This improves the detection of subtle changes in the mucosa of the pharynx and larynx that might suggest secondary effects from a sinus tumor. However, even the most advanced video laryngoscope cannot alter its fundamental anatomical path; it still visualizes the larynx and lower pharynx, not the sinuses. Its advantage lies in the clarity of what it does see, not in seeing new areas.