Views: 222 Author: Lake Publish Time: 2025-11-16 Origin: Site








Content Menu
● Understanding Isolation Gown Classifications
● Material Composition and Fluid Resistance
● Testing Standards and Performance Metrics
● Clinical Applications and Selection Criteria
● Limitations and Practical Considerations
● Comparative Analysis with Other Protective Garments
● Regulatory Framework and Quality Assurance
● Innovations and Future Developments
>> 1. Are all isolation gowns waterproof?
>> 2. How is the waterproof quality of isolation gowns tested?
>> 3. What level of isolation gown is needed for surgical procedures?
>> 4. Can isolation gowns be reused if they get wet?
>> 5. How do I choose the right isolation gown for waterproof needs?
The question of whether isolation gowns are waterproof touches upon fundamental aspects of personal protective equipment (PPE) in healthcare settings. Isolation gowns serve as critical barriers against fluid penetration and microbial transmission, with their waterproof capabilities varying significantly based on material composition, manufacturing standards, and intended use. Understanding the waterproof characteristics of isolation gowns requires examination of regulatory classifications, material science, and practical healthcare applications. This comprehensive analysis explores the fluid resistance properties of different types of isolation gowns, providing healthcare professionals, procurement specialists, and infection control practitioners with essential knowledge for appropriate selection and utilization of these vital protective garments in various clinical scenarios.

Isolation gowns are systematically classified based on their liquid barrier performance according to established standards. The ANSI/AAMI PB70 standard establishes four distinct levels of protection for isolation gowns, with each level representing specific capabilities against fluid penetration. Level 1 isolation gowns provide minimal fluid resistance, suitable for basic care and standard isolation precautions. Level 2 isolation gowns offer low fluid protection, appropriate for blood drawing procedures and suturing. Level 3 isolation gowns deliver moderate fluid resistance, ideal for arterial blood drawing and emergency room procedures. Level 4 isolation gowns provide the highest level of fluid protection, designed for surgical applications and scenarios involving large fluid volumes.
The classification system for isolation gowns enables healthcare facilities to match protective equipment with specific procedural risks. Not all isolation gowns are created equal in terms of waterproof capabilities, and understanding these distinctions is crucial for effective infection control. The waterproof characteristics of isolation gowns depend on multiple factors including fabric density, chemical treatments, and seam construction. Healthcare providers must recognize that the term "waterproof" in relation to isolation gowns exists on a spectrum rather than as an absolute characteristic, with different clinical situations requiring different levels of fluid protection.
The materials used in manufacturing isolation gowns directly influence their waterproof properties and overall protective capabilities. Traditional isolation gowns were primarily made from cotton or cotton-polyester blends, offering limited fluid resistance. Modern isolation gowns increasingly utilize nonwoven materials such as polypropylene, polyethylene, and SMS (spunbond-meltblown-spunbond) composites that provide enhanced fluid barrier properties. These advanced materials create isolation gowns with superior waterproof characteristics while maintaining breathability and comfort for healthcare workers.
The manufacturing processes for isolation gowns significantly impact their waterproof capabilities. Some isolation gowns undergo chemical treatments with fluorochemicals or other water-repellent finishes to enhance their fluid resistance. The density and structure of the materials used in isolation gowns determine their ability to prevent fluid penetration under various conditions. High-performance isolation gowns often feature laminated or coated fabrics that create effective barriers against fluid penetration while allowing moisture vapor transmission to maintain wearer comfort during extended use periods.
The waterproof capabilities of isolation gowns are rigorously tested according to standardized methodologies to ensure consistent performance. The American Association of Textile Chemists and Colorists (AATCC) test methods, particularly AATCC 42 and AATCC 127, evaluate the resistance of isolation gowns to water penetration under different conditions. These tests measure the ability of isolation gowns to withstand fluid exposure and provide quantitative data on their protective performance. The results from these standardized tests form the basis for classifying isolation gowns into different protection levels.
Additional testing protocols for isolation gowns include evaluating resistance to synthetic blood, viral penetration, and hydrostatic pressure. These comprehensive assessments ensure that isolation gowns meet the necessary requirements for their intended healthcare applications. The testing procedures simulate real-world conditions that isolation gowns might encounter in clinical settings, providing valuable information about their performance limitations and appropriate usage parameters. Understanding these test methods helps healthcare professionals interpret product specifications and make informed decisions when selecting isolation gowns for specific procedures.
The selection of appropriate isolation gowns based on waterproof requirements depends on the specific clinical procedure and anticipated exposure risks. Surgical isolation gowns, which typically represent the highest level of fluid protection, are essential in operating rooms where exposure to large volumes of blood and bodily fluids is expected. These isolation gowns are designed to provide comprehensive barrier protection, including reinforced critical zones that are most likely to encounter fluid exposure. The waterproof characteristics of surgical isolation gowns make them indispensable for maintaining sterility and protecting both patients and healthcare providers during invasive procedures.
For non-surgical applications, the choice of isolation gowns involves balancing waterproof requirements with other practical considerations. Standard isolation gowns used in medical wards, long-term care facilities, and outpatient settings may not require the same level of waterproof protection as surgical isolation gowns. However, these isolation gowns still need adequate fluid resistance to protect against unexpected exposures during routine patient care. Healthcare facilities must develop protocols that guide the selection of isolation gowns based on procedure-specific risk assessments, considering factors such as anticipated fluid volume, exposure duration, and potential pathogenicity of encountered fluids.
Despite advancements in material technology, all isolation gowns have limitations regarding their waterproof capabilities. The protective integrity of isolation gowns can be compromised by factors such as mechanical stress, chemical exposure, and improper donning or doffing procedures. Seams, closures, and interfaces with other PPE represent potential weak points in the waterproof barrier provided by isolation gowns. Healthcare workers must understand these limitations and follow proper protocols to maximize the protective benefits of isolation gowns during clinical use.
The duration of wear affects the waterproof performance of isolation gowns. Extended use of isolation gowns beyond their recommended time limits or exposure to multiple fluid challenges can diminish their protective properties. Additionally, environmental factors such as humidity and temperature may influence the performance of certain types of isolation gowns. Healthcare facilities must establish clear guidelines regarding the appropriate use and changing frequency of isolation gowns to ensure consistent protection. Regular training on the limitations and proper use of isolation gowns is essential for maintaining effective infection control practices.
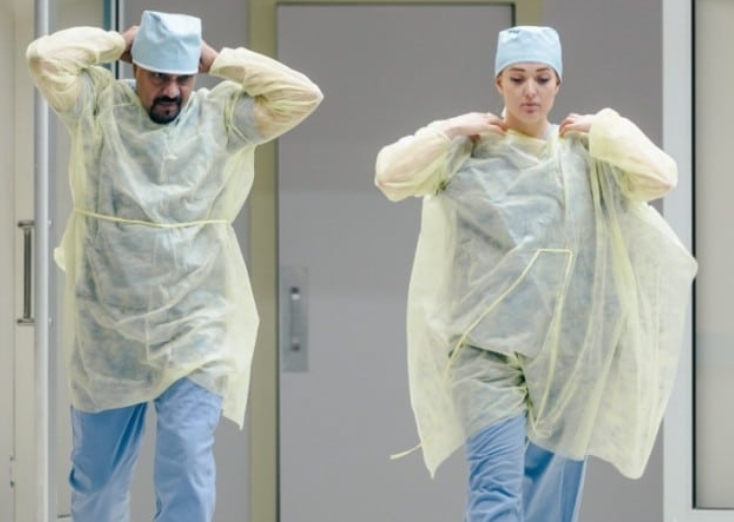
Understanding how isolation gowns compare to other types of protective garments provides valuable context for their waterproof capabilities. Surgical gowns, which represent a specialized category of isolation gowns, typically offer the highest level of fluid protection and are subject to more stringent testing requirements. Coveralls and aprons may provide alternative protection solutions in specific scenarios, though isolation gowns remain the standard for most healthcare applications requiring fluid resistance. The comparative analysis helps healthcare providers select the most appropriate protective equipment based on specific clinical needs and exposure risks.
The waterproof characteristics of isolation gowns must be considered in relation to their compatibility with other PPE components. The integration of isolation gowns with gloves, masks, and eye protection creates comprehensive protection systems that prevent fluid penetration at interface points. Modern isolation gowns often feature design elements that facilitate secure overlap with gloves and other protective equipment, enhancing the overall waterproof integrity of the PPE ensemble. This systems approach to protection ensures that isolation gowns function effectively as part of a complete barrier strategy in healthcare environments.
The manufacturing and performance standards for isolation gowns are governed by comprehensive regulatory frameworks that ensure consistent quality and protection levels. In the United States, the Food and Drug Administration (FDA) regulates isolation gowns as medical devices, requiring manufacturers to demonstrate compliance with established standards for fluid resistance and barrier protection. The ANSI/AAMI PB70 standard provides the foundational framework for classifying isolation gowns based on their liquid barrier performance, creating a standardized approach to product specification and selection.
Quality assurance processes for isolation gowns involve rigorous testing throughout the manufacturing cycle to verify consistent performance characteristics. Manufacturers of isolation gowns must implement quality management systems that monitor raw materials, production processes, and finished products to ensure compliance with regulatory requirements. Batch testing of isolation gowns provides additional verification of their waterproof capabilities and overall protective performance. These comprehensive quality assurance measures give healthcare providers confidence in the protective properties of the isolation gowns they utilize in clinical practice.
The evolution of isolation gowns continues with ongoing innovations aimed at enhancing waterproof capabilities while improving comfort and sustainability. Advanced material technologies are producing isolation gowns with superior fluid barrier properties through nanofiber coatings, smart fabric technologies, and improved laminate structures. These innovations enable the development of isolation gowns that provide exceptional waterproof protection while maintaining breathability and wearer comfort during extended procedures. The integration of sensor technologies into isolation gowns represents another emerging trend, potentially allowing real-time monitoring of fluid exposure and barrier integrity.
Sustainability considerations are increasingly influencing the development of isolation gowns with waterproof characteristics. Manufacturers are exploring eco-friendly materials and production processes that reduce environmental impact while maintaining protective performance. Reusable isolation gowns with durable waterproof coatings offer potential solutions to waste management challenges associated with single-use isolation gowns. These sustainable alternatives must demonstrate equivalent waterproof capabilities and barrier protection compared to conventional isolation gowns while withstanding repeated laundering and sterilization cycles. The future development of isolation gowns will likely balance advancements in waterproof technology with growing environmental concerns in healthcare sectors.
The waterproof capabilities of isolation gowns vary significantly based on their classification, material composition, and intended use. While no isolation gowns are completely waterproof in absolute terms, high-level isolation gowns provide substantial fluid resistance appropriate for most healthcare scenarios. The ANSI/AAMI PB70 classification system enables healthcare providers to select isolation gowns with appropriate waterproof characteristics based on specific procedural risks and exposure expectations. Understanding the limitations and proper use of isolation gowns is essential for maximizing their protective benefits in clinical environments.
Healthcare facilities must implement comprehensive protocols for the selection, use, and disposal of isolation gowns to ensure optimal infection control outcomes. The waterproof properties of isolation gowns represent just one aspect of their overall protective capability, which also includes resistance to microbial penetration, durability, and compatibility with other PPE components. As technology advances, the development of isolation gowns with enhanced waterproof characteristics, improved comfort, and reduced environmental impact will continue to evolve. Healthcare providers must stay informed about these developments to make appropriate decisions regarding the selection and utilization of isolation gowns in their practice settings.
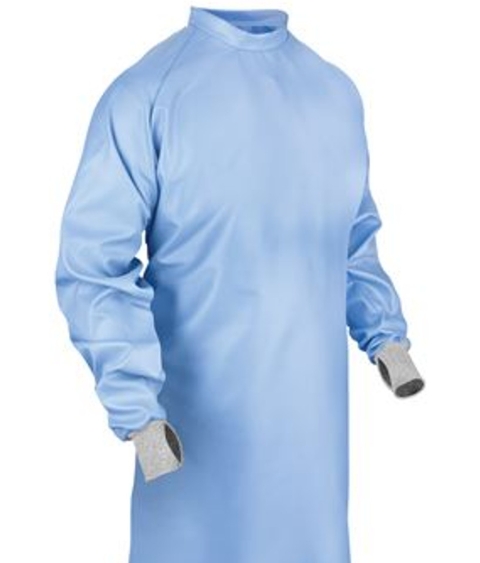
Not all isolation gowns are waterproof to the same degree. The fluid resistance of isolation gowns varies according to their protection level under the ANSI/AAMI PB70 classification system. Level 1 isolation gowns provide minimal fluid protection, while Level 4 isolation gowns offer the highest level of fluid resistance. The waterproof capabilities of isolation gowns depend on their material composition, construction, and intended use, with surgical isolation gowns typically providing the greatest fluid barrier protection.
The waterproof quality of isolation gowns is tested using standardized methods including AATCC 42 (Impact Penetration Test) and AATCC 127 (Hydrostatic Pressure Test). These tests measure the resistance of isolation gowns to water penetration under specific conditions. Additionally, isolation gowns may undergo testing with synthetic blood and viral penetration challenges to evaluate their barrier effectiveness in healthcare scenarios. The results from these tests determine the protection level of isolation gowns according to established classification standards.
Surgical procedures typically require Level 4 isolation gowns, which provide the highest level of fluid protection. These isolation gowns are designed to resist liquid penetration under the challenging conditions of surgical environments, where exposure to blood and bodily fluids is anticipated. Surgical isolation gowns feature reinforced critical zones and comprehensive barrier properties to protect both the surgical team and the patient. The selection of appropriate isolation gowns for surgical applications should be based on the specific procedure type and anticipated fluid exposure risks.
Isolation gowns are generally designed for single use and should not be reused, especially if they have become wet or contaminated. The protective barrier of isolation gowns can be compromised by fluid exposure, and reusing them may increase infection transmission risks. Most isolation gowns are intended for disposal after use, though some reusable options exist that require proper laundering and reprocessing between uses. Healthcare facilities should establish clear protocols regarding the single-use nature of isolation gowns and proper disposal procedures after contamination.
Choosing the right isolation gown for waterproof needs involves assessing the specific clinical procedure, anticipated fluid exposure, and required protection level. Consult the ANSI/AAMI PB70 classification system when selecting isolation gowns, matching the protection level to the procedural risks. Level 2 or 3 isolation gowns may suffice for procedures with low to moderate fluid exposure, while Level 4 isolation gowns are necessary for high-fluid situations. Additionally, consider factors such as comfort, breathability, and compatibility with other PPE when selecting isolation gowns for specific healthcare applications.
[1] https://www.fda.gov/medical-devices/personal-protective-equipment-infection-control/isolation-gowns
[2] https://www.cdc.gov/niosh/npptl/topics/protectiveclothing/default.html
[3] https://www.aami.org/docs/default-source/standards-library/ansi_aami_pb70.pdf
[4] https://www.astm.org/Standards/F2407.htm
[5] https://www.fda.gov/medical-devices/medical-device-databases/code-classification-database
[6] https://www.cdc.gov/infectioncontrol/guidelines/isolation/index.html