







Content Menu
● Understanding Isolation Gown Types and Their Implications for Removal
● Preparation for Isolation Gown Removal
● Step-by-Step Removal Procedure for Tied Isolation Gowns
● Technique for Disposing of Contaminated Isolation Gowns
● Removal of Isolation Gown as Part of Full PPE Doffing Sequence
● Special Considerations for Different Clinical Scenarios
● Common Errors in Isolation Gown Removal and How to Avoid Them
● Training and Competency Assessment for Proper Isolation Gown Removal
● Environmental Considerations and Sustainability Aspects
>> 1. What is the correct sequence for removing an isolation gown when wearing full PPE?
>> 2. Why is it important to follow a specific technique when removing an isolation gown?
>> 3. How should I handle an isolation gown that is heavily soiled or contaminated?
>> 4. Can isolation gowns be reused, and how does this affect removal technique?
>> 5. What should I do if I make a mistake during isolation gown removal?
The proper removal of an isolation gown represents a critical procedure in infection prevention and control protocols within healthcare settings. Understanding the correct technique for doffing (removing) an isolation gown is equally as important as proper donning (putting on) procedures, as contamination most frequently occurs during the removal process. The isolation gown serves as a crucial barrier against infectious materials, but its protective function can be compromised if removed incorrectly, potentially leading to self-contamination or transmission of pathogens to other surfaces or individuals. This comprehensive guide examines the systematic approach to isolation gown removal, addressing different types of gowns, various clinical scenarios, and the essential safety considerations that healthcare workers must understand to maintain both personal protection and environmental safety. Mastering the technique of isolation gown removal requires not only knowledge of the sequential steps but also an understanding of the principles underlying these procedures.
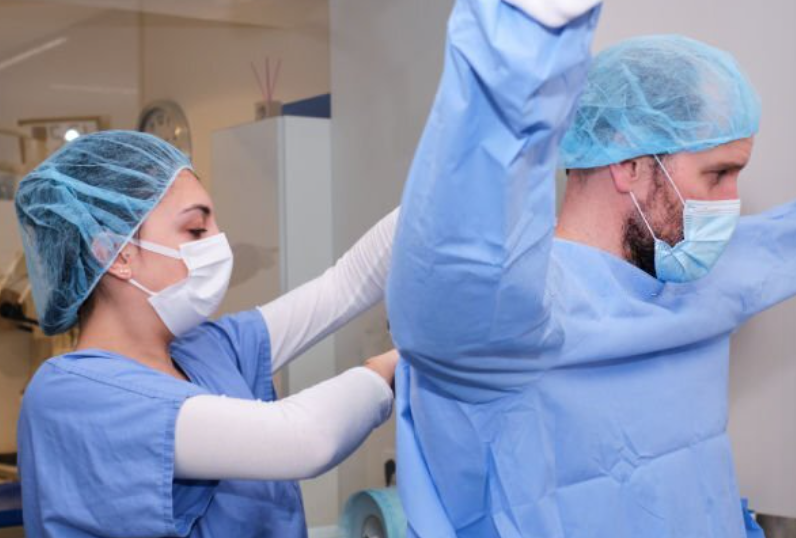
The removal procedure for an isolation gown varies depending on the specific type of gown being used. Disposable isolation gown typically feature tie closures at the neck and waist, with most designed for single-use before disposal. Reusable isolation gown generally feature more durable closures such as snaps or buttons and are designed to withstand multiple laundering cycles. The material composition of the isolation gown also influences removal techniques, with fluid-resistant and impermeable isolation gown requiring more careful handling due to potential contamination on the outer surface.
The design features of an isolation gown directly impact the removal process. Open-backed isolation gown with tie closures require careful unfastening while maintaining minimal contact with the outer surface. Full-wrap isolation gown that provide complete coverage typically feature longer ties that must be managed systematically during removal. Understanding the specific fastening mechanisms on an isolation gown - whether ties, snaps, buttons, or hook-and-loop closures - is essential for planning the removal sequence. Additionally, the level of protection provided by the isolation gown (as determined by standards such as ANSI/AAMI PB70) may influence removal caution, with higher protection level gowns used in more hazardous situations requiring more meticulous removal techniques.
Proper preparation is essential before initiating the removal of an isolation gown. The first step involves identifying an appropriate location for isolation gown removal, ideally a dedicated area with sufficient space to perform the procedure without touching environmental surfaces or other individuals. If the isolation gown removal will occur in a patient room, position yourself away from patient care areas and any clean surfaces. Before touching the isolation gown, perform hand hygiene if hands are visibly soiled, though thorough hand hygiene typically follows isolation gown removal in the complete sequence of personal protective equipment (PPE) removal.
Mental rehearsal of the isolation gown removal sequence can enhance performance, particularly in high-stress situations. Visualize each step of the process, from initial unfastening to final disposal or placement in a laundry container. If working with an observer or buddy during isolation gown removal, establish clear communication about their role in identifying potential contamination risks. Ensure that appropriate waste receptacles or laundry hampers are positioned conveniently before beginning isolation gown removal. This preparatory phase, though brief, establishes the foundation for safe and systematic isolation gown removal.
The removal of a tied isolation gown follows a specific sequence designed to minimize contamination risk. Begin the isolation gown removal process by unfastening the waist ties. Using one gloved hand, locate the knot or bow at the waist and untie it. If the ties are particularly tight or difficult to manage with gloved hands, a gentle pull on the free ends may loosen the knot. Avoid excessive force during this step of isolation gown removal, as aggressive pulling may cause the gown to tear or generate aerosols from contaminated surfaces.
After unfastening the waist tie, proceed to the neck area of the isolation gown. With both hands still gloved, reach to the neckline and untie the neck ties. Some isolation gown designs feature a single tie at the neck, while others may have snaps or buttons in addition to or instead of ties. Once both waist and neck fastenings are released, grasp the isolation gown at the shoulders and pull forward gently, allowing the gown to fall away from the body. During this phase of isolation gown removal, touch only the inside surface of the gown, which is considered clean. As the isolation gown comes away from the body, fold or roll it inward, containing the contaminated exterior surface within the bundle.
Proper disposal of a contaminated isolation gown represents a critical component of the removal process that prevents environmental contamination. After successfully removing the isolation gown using the appropriate technique, transport the folded or rolled gown directly to the appropriate waste receptacle. For disposable isolation gown, this typically means a regular waste container for non-hazardous use or a biohazard bag if the gown is contaminated with blood or body fluids. When approaching the waste container during isolation gown disposal, avoid touching the container with any part of the gown or your gloves.
Position yourself close to the disposal container before releasing the isolation gown to minimize the distance it falls. Gently place the isolation gown into the receptacle, taking care not to generate aerosols or disperse contaminants. If the isolation gown disposal requires opening a container lid, use a foot pedal if available, or have an assistant open the lid. Never compress or push down an isolation gown already in a disposal container, as this may force contaminants through the bag or create aerosols. After successful isolation gown disposal, proceed immediately to hand hygiene before any other patient or environmental contact.
The isolation gown removal typically occurs as part of a comprehensive PPE doffing sequence rather than as an isolated procedure. In most protocols, the isolation gown is removed after other PPE components, though the exact sequence may vary based on the specific combination of PPE worn and the nature of the contamination risk. When wearing gloves with an isolation gown, the standard sequence involves removing gloves first, followed by the isolation gown, though some protocols recommend removing the isolation gown with gloves still on, particularly when the gown has extended cuffs that cover the glove-wrist interface.
When the isolation gown is worn in combination with a face shield or goggles, the face protection is typically removed after the isolation gown but before respiratory protection. If a respirator is worn, it is usually removed after the isolation gown but before exiting the patient care area. Understanding where isolation gown removal fits within the complete PPE doffing sequence is essential for maintaining protection throughout the process. Healthcare facilities should establish and train on standardized sequences for isolation gown removal within the context of full PPE protocols to ensure consistency and safety across all personnel.
The technique for isolation gown removal may require modification based on specific clinical scenarios and contamination risks. When removing an isolation gown after caring for patients with contact precautions, additional caution is warranted due to the higher risk of environmental contamination. In situations where the isolation gown is visibly contaminated with substantial blood, body fluids, or other potentially infectious materials, a more deliberate approach to isolation gown removal is necessary, potentially including a double-gloving technique to provide an additional layer of protection during the removal process.
For aerosol-generating procedures, isolation gown removal should occur in an anteroom or adjacent area rather than immediately within the patient environment. When dealing with extensively drug-resistant organisms, some protocols may recommend discarding the isolation gown within the patient room rather than transporting it even short distances. In surgical settings, the isolation gown removal technique differs significantly, often involving a specific turning motion and having an assistant release ties from behind. Understanding these scenario-specific modifications to standard isolation gown removal procedures enhances both safety and protocol compliance across diverse clinical situations.
Several common errors can compromise the safety of isolation gown removal, potentially leading to self-contamination or environmental spread of pathogens. One frequent mistake is failing to untie both the neck and waist fastenings before attempting to remove the isolation gown, which can cause tearing or excessive manipulation of the gown. Another common error during isolation gown removal is touching the outside contaminated surface with bare hands during the removal process, typically occurring when individuals grasp the exterior of the gown rather than the interior clean surface.
Improper disposal technique represents another category of errors in isolation gown removal, including tossing the gown toward a receptacle from a distance rather than placing it gently, or missing the receptacle entirely. Some healthcare workers commit the error of removing the isolation gown too early in the PPE doffing sequence, potentially contaminating other PPE components or skin surfaces. Additionally, failing to perform hand hygiene immediately after isolation gown removal negates much of the protection gained by proper technique. Awareness of these common errors enables healthcare workers to implement corrective strategies during isolation gown removal, such as mental checkpoints, peer observation, and adherence to trained protocols.
Effective training methodologies are essential for ensuring healthcare workers can perform isolation gown removal correctly and consistently. Simulation-based training provides the optimal approach for teaching isolation gown removal techniques, allowing learners to practice the sequence repeatedly in a low-risk environment. Training programs should incorporate different types of isolation gown to ensure proficiency across the various designs and fastening systems that healthcare workers may encounter. Visual aids such as posters demonstrating the step-by-step process of isolation gown removal can serve as valuable references when displayed in appropriate locations.
Competency assessment for isolation gown removal should evaluate both the technical sequence and the underlying principles of infection prevention. Assessment tools for isolation gown removal competency typically include checklists that specify each critical step, with particular emphasis on aspects that prevent self-contamination. Regular competency validation ensures that healthcare workers maintain proficiency in isolation gown removal, with frequency determined by institutional policy and regulatory requirements. Just-in-time training immediately before isolation gown use in high-risk situations can reinforce proper technique. Effective training and assessment programs for isolation gown removal contribute significantly to infection prevention outcomes in healthcare settings.
The environmental impact of isolation gown use and disposal has gained increasing attention in healthcare sustainability initiatives. The disposal process for single-use isolation gown contributes to the substantial waste stream generated by healthcare facilities, with implications for landfill capacity and environmental pollution. Reusable isolation gown systems offer an alternative approach that reduces waste but requires energy, water, and chemical resources for laundering. The removal procedure for reusable isolation gown differs from disposable versions, often involving placement in specific laundry containers rather than waste receptacles.
During isolation gown removal of reusable models, healthcare workers must ensure proper containment of the contaminated gown to prevent environmental contamination during transport to laundry facilities. The technique for isolation gown removal should minimize shaking or agitation that could disperse contaminants into the air. Some facilities have implemented innovative approaches to isolation gown sustainability, including recycling programs for certain types of disposable gowns and selection of gowns with reduced environmental impact. Balancing infection prevention requirements with environmental considerations presents an ongoing challenge in isolation gown selection, use, and removal protocols.
The proper removal of an isolation gown represents a fundamental infection prevention skill that all healthcare workers must master to protect themselves, their patients, and the healthcare environment. The technique for isolation gown removal, when performed correctly, prevents the transmission of pathogens that may have contaminated the gown's exterior during patient care activities. This comprehensive guide has detailed the systematic approach to isolation gown removal, including preparation, step-by-step procedures, disposal methods, and integration within complete PPE protocols. Understanding the principles underlying isolation gown removal - particularly the concept of clean versus contaminated surfaces - enables healthcare workers to adapt the technique to various gown designs and clinical scenarios. Regular training, competency assessment, and adherence to established protocols ensure that isolation gown removal consistently achieves its intended protective function. As healthcare continues to evolve, with new materials, gown designs, and infection challenges emerging, the fundamental importance of proper isolation gown removal remains constant as a cornerstone of infection prevention practice.
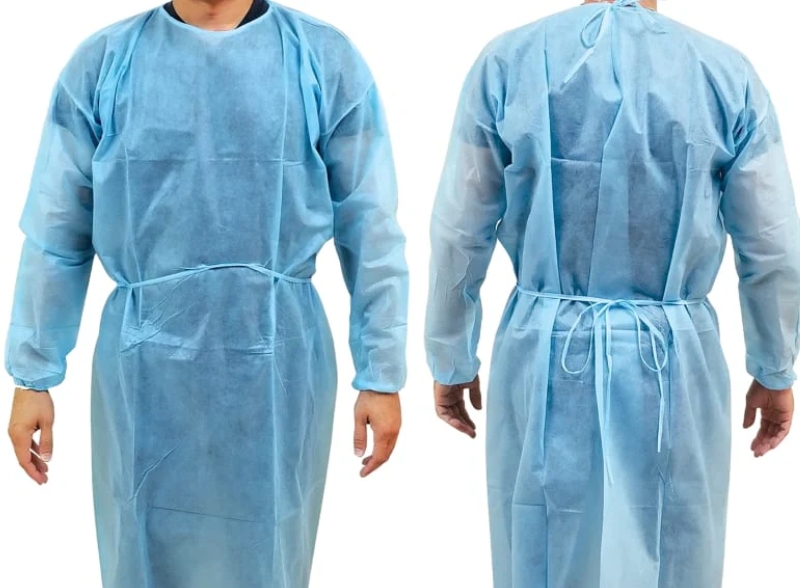
The isolation gown removal typically occurs after gloves but before face protection in the standard PPE removal sequence. The complete sequence generally involves: (1) removing and disposing of gloves properly, (2) performing hand hygiene, (3) removing the isolation gown by unfastening ties and pulling away from the body while touching only the inside surface, (4) disposing of the isolation gown appropriately, (5) removing face protection, (6) performing hand hygiene again. However, specific sequences may vary based on institutional protocol and the type of isolation gown and additional PPE being used.
Following a specific technique for isolation gown removal is crucial because the exterior surface of the gown is considered contaminated after use. Proper isolation gown removal technique prevents healthcare workers from touching the contaminated exterior with their bare hands or clothing, thereby reducing the risk of self-contamination. The systematic approach to isolation gown removal also minimizes the generation of aerosols that could disperse pathogens into the environment. Additionally, consistent isolation gown removal technique ensures that the protective function of the gown is maintained throughout the doffing process rather than compromised at the final stage of use.
When dealing with a heavily soiled or contaminated isolation gown, exercise additional caution during the removal process. Before beginning isolation gown removal, ensure you have appropriate disposal materials readily available, including a biohazard bag if required by your facility's protocol. Consider double-gloving before patient care if heavy contamination is anticipated, as this provides an additional protective layer during isolation gown removal. When removing a heavily contaminated isolation gown, move more deliberately and avoid any shaking or aggressive manipulation that might dislodge contaminants. After removal of a heavily soiled isolation gown, perform hand hygiene particularly thoroughly, including attention to fingernails and all hand surfaces.
Most isolation gown used in healthcare settings are designed for single use and should not be reused. However, some facilities utilize reusable isolation gown made of launderable materials. The removal technique for a reusable isolation gown differs in the disposal step - instead of placing the gown in a waste receptacle, it should be placed in a designated laundry bag or container. The actual removal sequence for a reusable isolation gown is similar to disposable versions, with careful attention to containing the contaminated exterior during removal. Facilities using reusable isolation gown must provide clear protocols for their proper removal and containment to prevent environmental contamination during transport to laundry facilities.
If you recognize a mistake during isolation gown removal, such as accidentally touching the contaminated exterior surface, immediately stop the removal process and perform hand hygiene. If the isolation gown removal error involves significant contamination of your skin or clothing, follow your facility's protocol for exposure management, which may include skin cleansing, changing of clothing, and reporting the incident to your supervisor or occupational health department. After addressing any immediate contamination concerns, don a new isolation gown if you still require protection, or complete the removal process with heightened attention to technique. Documentation of isolation gown removal errors can help identify systematic issues that might be addressed through additional training or protocol modifications.