







Content Menu
● Understanding Bronchoscope Design and Cleaning Challenges
>> Complex Instrument Architecture
● Immediate Post-Procedure Cleaning
● Automated Cleaning and Disinfection
>> Automated Endoscope Reprocessors
>> Chemical Compatibility and Selection
● Drying and Storage Protocols
>> Appropriate Storage Conditions
● Quality Assurance and Monitoring
● Staff Training and Competency
>> Comprehensive Training Programs
>> Competency Validation and Assessment
● FAQ
>> 1. Why is bronchoscope cleaning so complicated?
>> 2. How soon after a procedure should bronchoscope cleaning begin?
>> 3. What is the purpose of leak testing a bronchoscope before cleaning?
>> 4. Can automated reprocessors completely clean a bronchoscope without manual cleaning?
>> 5. How long can a properly cleaned bronchoscope be stored before it needs reprocessing?
The proper cleaning of a bronchoscope represents one of the most critical aspects of infection control in pulmonary medicine and critical care. Achieving true cleanliness of a bronchoscope involves a meticulous, multi-step process designed to remove all organic material and microorganisms from these complex medical instruments. The intricate design of a bronchoscope, with its long narrow channels, movable parts, and delicate components, presents unique challenges for effective cleaning. Understanding and implementing proper bronchoscope cleaning protocols is essential for preventing healthcare-associated infections, maintaining equipment functionality, and ensuring patient safety during bronchoscopic procedures.
The consequences of inadequate bronchoscope cleaning can be severe, with numerous documented cases of infection transmission linked to improperly processed bronchoscopes. The complex internal structure of a bronchoscope can harbor pathogens despite apparent visual cleanliness, making standardized cleaning protocols absolutely essential. This comprehensive guide examines the detailed steps, best practices, and quality assurance measures necessary to ensure proper bronchoscope cleaning in healthcare settings.

The modern bronchoscope represents a sophisticated medical instrument with numerous components that require careful attention during cleaning. A standard flexible bronchoscope contains an insertion tube housing fiber optic bundles or digital imaging sensors, light transmission fibers, a working channel for instrument passage, and deflection control mechanisms. The working channel of the bronchoscope typically measures only 2-3 mm in diameter, creating significant challenges for effective cleaning and debris removal. The intricate design of the bronchoscope includes multiple hard-to-reach areas where blood, mucus, and other organic material can accumulate if not properly cleaned.
The control section of the bronchoscope contains valves, ports, and connections that require meticulous cleaning to prevent biofilm formation. The distal tip of the bronchoscope includes the objective lens, light guide lens, and working channel opening—all requiring careful cleaning to maintain optical clarity and prevent contamination. Understanding this complex architecture is essential for effective bronchoscope cleaning, as each component presents unique cleaning challenges and requirements. The design complexity of the bronchoscope necessitates a systematic approach to ensure all surfaces and channels receive proper attention during the cleaning process.
The internal channels of a bronchoscope provide ideal environments for biofilm formation if not properly cleaned. Biofilms are structured communities of microorganisms encased in a protective matrix that can adhere to the internal surfaces of the bronchoscope channels. Once established, biofilms are extremely difficult to remove and can serve as persistent sources of pathogen transmission between patients. The narrow working channel of the bronchoscope is particularly vulnerable to biofilm formation due to its small diameter and the difficulty of achieving mechanical cleaning action within this confined space.
Biofilms in a bronchoscope can compromise subsequent disinfection or sterilization steps by protecting microorganisms from chemical germicides. Even apparently clean bronchoscope channels may harbor biofilms that are not visible to the naked eye. Preventing biofilm formation requires prompt and thorough cleaning of the bronchoscope immediately after each use, before organic material has time to dry and adhere to channel surfaces. Understanding the risk of biofilm development underscores the importance of meticulous bronchoscope cleaning protocols in preventing healthcare-associated infections.
The cleaning process for a bronchoscope should begin immediately after the procedure concludes, while the instrument is still at the patient's bedside. This initial cleaning step is crucial for preventing the drying of organic material inside the bronchoscope channels, which can make subsequent cleaning more difficult. The bedside cleaning of the bronchoscope involves wiping the exterior with a soft cloth moistened with enzymatic detergent solution and flushing the working channel with the same solution. This initial bronchoscope cleaning step removes gross contamination and keeps organic material hydrated until more thorough cleaning can be performed.
During bedside cleaning, the bronchoscope should be transported carefully to prevent damage to the delicate insertion tube. The bronchoscope should be placed in a designated container labeled with biohazard symbols for transport to the cleaning area. Healthcare personnel should wear appropriate personal protective equipment during bedside bronchoscope cleaning and transport to minimize exposure to potentially infectious material. This prompt initial cleaning of the bronchoscope represents the first and perhaps most critical step in the reprocessing sequence, setting the stage for effective subsequent processing.
Before immersion cleaning, every bronchoscope must undergo leak testing to identify any damage that could allow fluid penetration into the internal components. The leak tester is connected to the bronchoscope according to manufacturer instructions, and the instrument is pressurized while submerged in water. The entire bronchoscope, especially the bending section and control area, should be carefully observed for a minimum of 30 seconds while applying gentle angulation to the insertion tube. Any stream of bubbles emerging from the bronchoscope indicates a breach that requires repair before the instrument can be safely immersed in cleaning solutions.
Leak testing the bronchoscope serves two critical purposes: it identifies damage that could compromise patient safety during procedures, and it prevents fluid intrusion that could damage the internal components of the bronchoscope during cleaning. A bronchoscope that fails leak testing must be removed from service immediately and sent for repair. Documentation of each leak test performed on the bronchoscope provides important quality assurance data and helps track instrument integrity over time. This essential safety step protects both patients and the significant financial investment represented by each bronchoscope.

The manual cleaning of the bronchoscope exterior requires meticulous attention to all external surfaces. Using a soft, lint-free cloth or sponge moistened with enzymatic detergent solution, all external surfaces of the bronchoscope should be thoroughly wiped, paying particular attention to the distal tip, bending section, and control body. The bronchoscope should be carefully inspected during cleaning to ensure all visible soil is removed from crevices, ridges, and the area around control knobs. A small soft brush may be used to clean difficult-to-reach areas of the bronchoscope exterior, taking care not to damage delicate components.
All detachable parts of the bronchoscope, such as suction valves and channel caps, should be removed according to manufacturer instructions and cleaned separately. These bronchoscope components often have intricate designs that can harbor organic material if not properly cleaned. The distal tip of the bronchoscope requires special attention during external cleaning, as the lenses and channel openings can accumulate debris that may compromise visualization or instrument function. Throughout the external cleaning process, the bronchoscope should be handled gently to prevent damage to the fragile insertion tube and distal tip.
The internal channels of the bronchoscope represent the most challenging aspect of the cleaning process due to their narrow diameter and limited accessibility. All internal channels of the bronchoscope must be brushed with appropriately sized cleaning brushes specifically designed for each channel type. The brush should be passed completely through each bronchoscope channel multiple times, rotating the brush during insertion and withdrawal to ensure all internal surfaces are contacted. After brushing, each channel of the bronchoscope should be flushed with enzymatic detergent solution using channel-specific adapters to ensure adequate flow through all lumens.
The working channel of the bronchoscope typically requires the most attention during internal cleaning, as it is exposed to the greatest amount of organic material during procedures. Specialized brushes designed specifically for the bronchoscope working channel should be used according to manufacturer recommendations regarding brush size and technique. After brushing, the bronchoscope channels should be flushed with copious amounts of enzymatic detergent solution until the effluent runs clear, indicating removal of all visible soil. This thorough internal cleaning of the bronchoscope is essential for preventing biofilm formation and ensuring effective disinfection.
Automated endoscope reprocessors (AERs) provide standardized cleaning and disinfection for bronchoscope instruments after manual cleaning has been completed. These specialized systems connect to all channels of the bronchoscope and cycle measured amounts of cleaning and disinfecting solutions through the instrument according to programmed parameters. The use of an AER for bronchoscope reprocessing enhances consistency and reduces variability compared to manual processing methods. However, it is crucial to understand that AERs are designed to disinfect a properly cleaned bronchoscope, not to clean a dirty one.
When using an AER for bronchoscope reprocessing, healthcare personnel must ensure proper connection of all bronchoscope channels according to manufacturer instructions. The AER must be used with cleaning and disinfecting solutions approved by both the AER manufacturer and the bronchoscope manufacturer. Regular maintenance and testing of the AER are essential to ensure proper function during bronchoscope reprocessing. While AERs provide valuable standardization, they do not eliminate the need for meticulous manual cleaning of the bronchoscope before automated processing.
The selection of appropriate cleaning and disinfecting chemicals for bronchoscope reprocessing requires careful consideration of material compatibility and efficacy. Enzymatic detergents used for bronchoscope cleaning should be specifically formulated for endoscope reprocessing and compatible with bronchoscope materials. These detergents break down organic material through enzymatic action, facilitating soil removal from the complex internal channels of the bronchoscope. The enzymatic detergent solution should be prepared according to manufacturer instructions regarding concentration and temperature to ensure optimal effectiveness.
High-level disinfectants used for bronchoscope reprocessing must be selected based on their efficacy against relevant microorganisms, material compatibility with the bronchoscope, and safety profile for healthcare workers. Common disinfectants for bronchoscope reprocessing include ortho-phthalaldehyde (OPA), peracetic acid, and glutaraldehyde-based formulations. Each disinfectant has specific advantages and limitations regarding contact time, material compatibility, and potential for residual toxicity. The selection of chemicals for bronchoscope reprocessing should follow manufacturer recommendations and be supported by institutional policies based on current evidence and guidelines.
Thorough drying of the bronchoscope after cleaning and disinfection is essential for preventing microbial growth during storage. All internal channels of the bronchoscope must be purged with forced air using specifically designed drying systems or clean, filtered compressed air. The bronchoscope should be hung vertically in a dedicated drying cabinet to facilitate complete drainage and evaporation of residual moisture. The drying time for a bronchoscope should follow manufacturer recommendations, typically requiring a minimum of 30 minutes of forced air flushing followed by additional air-drying time.
The external surfaces of the bronchoscope should be carefully dried with a clean, lint-free cloth before storage. Particular attention should be paid to the distal tip, control body, and channel ports of the bronchoscope to ensure no moisture remains in crevices or around valves. Incomplete drying of the bronchoscope creates an environment conducive to microbial proliferation, potentially contaminating the instrument before its next use. Proper drying of the bronchoscope represents the final critical step in the reprocessing sequence before storage.
Proper storage of the bronchoscope after cleaning and drying is essential for maintaining its cleanliness until the next use. The bronchoscope should be stored in a dedicated, well-ventilated storage cabinet designed specifically for endoscope storage. The storage cabinet for bronchoscope instruments should protect from dust, moisture, and physical damage while allowing air circulation around the stored instruments. The bronchoscope should be hung vertically in a relaxed, non-coiled position to prevent damage to the insertion tube and internal components.
The storage environment for bronchoscope instruments should maintain appropriate temperature and humidity levels to prevent microbial growth and material degradation. Storage areas for bronchoscope equipment should be located away of sinks, drains, and other potential sources of contamination. Each bronchoscope should be stored separately to prevent contact between instruments that could cause damage or transfer contamination. Proper labeling and tracking of storage times for each bronchoscope help ensure rotation and appropriate use based on reprocessing dates.
Comprehensive documentation is essential for quality assurance in bronchoscope cleaning and reprocessing. Each bronchoscope reprocessing cycle should be documented with specific information including the bronchoscope identification number, date and time of reprocessing, individual performing the reprocessing, lot numbers of chemicals used, and any deviations from standard protocols. This documentation for bronchoscope reprocessing provides an auditable trail for quality assurance purposes and facilitates tracking in the event of infection control concerns.
In addition to process documentation, regular maintenance records for each bronchoscope should be maintained, including leak test results, repair history, and performance issues noted during procedures. Documentation of staff training and competency validation for bronchoscope reprocessing provides evidence of qualified personnel performing these critical tasks. This comprehensive documentation approach for bronchoscope management supports quality improvement initiatives and regulatory compliance while ensuring patient safety.
Some healthcare facilities implement microbiological surveillance programs to monitor the effectiveness of bronchoscope cleaning and reprocessing protocols. These programs typically involve periodic culturing of processed bronchoscope channels to detect residual microbial contamination. The specific approach to bronchoscope surveillance culturing varies between institutions, with some facilities testing all bronchoscopes regularly and others testing on a rotating schedule or in response to specific concerns.
When implementing bronchoscope surveillance culturing, facilities must establish clear protocols for sample collection, transportation, and interpretation of results. Action thresholds for bronchoscope culturing results should be established in advance, with defined responses for various levels of microbial recovery. While not universally implemented, bronchoscope surveillance culturing can provide valuable data on reprocessing effectiveness and identify potential issues before they lead to patient infections. The decision to implement bronchoscope culturing should be based on institutional risk assessment and available resources.
Effective bronchoscope cleaning requires comprehensive training programs for all personnel involved in the reprocessing workflow. Training for bronchoscope reprocessing should include both theoretical knowledge and hands-on practical skills. The theoretical component should cover the basic principles of infection control, the specific design features of the bronchoscope models used in the facility, and the step-by-step reprocessing protocols. Understanding the "why" behind each bronchoscope cleaning step enhances compliance with established protocols.
Hands-on training for bronchoscope reprocessing should allow practice with actual instruments or realistic training models under the supervision of experienced preceptors. Trainees should demonstrate competency in each aspect of bronchoscope reprocessing, including bedside cleaning, leak testing, manual cleaning, automated reprocessor operation, and proper storage. Training programs for bronchoscope reprocessing should be documented for each staff member, with records maintained as evidence of competency. This comprehensive approach to bronchoscope reprocessing training ensures that all personnel understand their critical role in patient safety.
Regular competency validation is essential for maintaining high standards in bronchoscope cleaning and reprocessing. Healthcare facilities should establish periodic competency assessments for all personnel involved in bronchoscope reprocessing, typically conducted annually or when new equipment or protocols are introduced. Competency assessment for bronchoscope reprocessing should include both knowledge-based testing and direct observation of technical skills during actual reprocessing activities.
The competency assessment for bronchoscope reprocessing should evaluate understanding of manufacturer instructions, proper use of cleaning equipment and chemicals, adherence to infection control practices, and appropriate documentation. Staff performing bronchoscope reprocessing should also demonstrate knowledge of troubleshooting common problems and recognizing when a bronchoscope requires repair or specialized handling. This ongoing competency validation for bronchoscope reprocessing ensures that staff maintain the necessary skills and knowledge to perform these critical tasks effectively and safely.
The proper cleaning of a bronchoscope represents a complex, multi-step process that demands meticulous attention to detail and adherence to established protocols. From immediate bedside cleaning through thorough manual cleaning, disinfection, drying, and proper storage, each step in the bronchoscope reprocessing sequence plays a vital role in ensuring patient safety and instrument functionality. The intricate design of the bronchoscope, with its narrow channels and delicate components, presents unique challenges that require specialized knowledge, equipment, and techniques for effective cleaning.
Healthcare facilities must prioritize bronchoscope cleaning through comprehensive staff training, robust quality assurance programs, and strict adherence to manufacturer guidelines and evidence-based practices. The consequences of inadequate bronchoscope cleaning can be severe, including healthcare-associated infections, equipment damage, and regulatory sanctions. By implementing and maintaining rigorous bronchoscope cleaning protocols, healthcare organizations can ensure the safety of bronchoscopic procedures while protecting their significant investment in these sophisticated medical instruments. The commitment to proper bronchoscope cleaning ultimately reflects the broader commitment to patient safety and quality healthcare delivery.
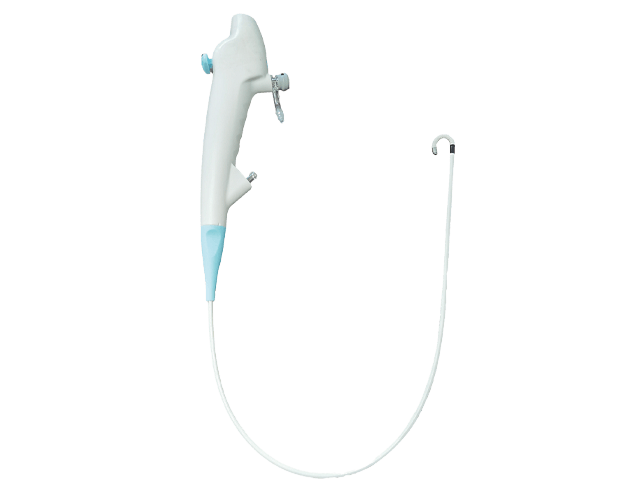
Bronchoscope cleaning is particularly complicated due to the instrument's complex design and multiple hard-to-reach areas. A standard bronchoscope contains long narrow channels, movable parts, and delicate components that can harbor microorganisms if not thoroughly cleaned. The working channel of the bronchoscope typically measures only 2-3 mm in diameter, making mechanical cleaning challenging. Additionally, the bronchoscope has multiple ports, valves, and connections that require meticulous attention during cleaning. The risk of biofilm formation in bronchoscope channels further complicates cleaning, as established biofilms can protect microorganisms from disinfectants. These design complexities necessitate a multi-step cleaning process with specialized equipment and techniques to ensure all surfaces of the bronchoscope are properly cleaned.
Bronchoscope cleaning should begin immediately after the procedure concludes, ideally at the patient's bedside. Prompt initiation of bronchoscope cleaning is crucial for preventing the drying of organic material inside the instrument's channels. When organic material dries inside a bronchoscope, it becomes more difficult to remove and can facilitate biofilm formation. The initial bedside cleaning of the bronchoscope involves wiping the exterior with enzymatic detergent and flushing the working channel with the same solution. This immediate bronchoscope cleaning step keeps organic material hydrated and facilitates more thorough cleaning once the instrument reaches the dedicated reprocessing area. Delaying bronchoscope cleaning, even for short periods, can compromise the effectiveness of subsequent cleaning and disinfection steps.
Leak testing a bronchoscope before cleaning serves two critical purposes: it identifies damage that could compromise patient safety, and it prevents fluid intrusion that could damage the instrument during cleaning. The leak test involves pressurizing the bronchoscope and submerging it in water to check for air bubbles indicating breaches in the instrument's integrity. A bronchoscope with a leak could allow fluid to penetrate internal components during immersion cleaning, causing extensive damage to delicate optics and electronics. Additionally, a compromised bronchoscope could potentially injure patients during procedures if internal components are damaged. Regular leak testing of every bronchoscope before each cleaning cycle is essential for both equipment protection and patient safety.
No, automated reprocessors cannot completely clean a bronchoscope without thorough manual cleaning first. Automated endoscope reprocessors (AERs) are designed to disinfect a properly cleaned bronchoscope, not to clean a dirty one. Manual cleaning of the bronchoscope is essential for removing organic material that could shield microorganisms from disinfectants used in automated reprocessors. The mechanical action of brushing the bronchoscope channels and wiping the external surfaces is necessary to disrupt and remove biofilms and adherent debris. Attempting to process a soiled bronchoscope in an AER without proper manual cleaning will result in inadequate reprocessing and potential infection risks. Manual cleaning remains an indispensable step in bronchoscope reprocessing, even when using advanced automated systems.
A properly cleaned, disinfected, and thoroughly dried bronchoscope can typically be stored for up to 5-7 days before requiring reprocessing, though specific storage duration should follow manufacturer recommendations and institutional policies. The storage time for a bronchoscope depends on multiple factors, including the storage environment, drying completeness, and packaging methods. Bronchoscope instruments stored in dedicated ventilated cabinets that protect from dust and moisture may maintain their processed state longer than those stored in suboptimal conditions. Some facilities implement more conservative storage timelines for bronchoscope instruments, particularly in high-risk settings. Regardless of the specified storage duration, a bronchoscope should always be visually inspected before use and reprocessed if any concerns about its cleanliness or integrity arise.
[1] https://www.fda.gov/medical-devices/reprocessing-medical-devices/bronchoscopes-reprocessing
[2] https://www.cdc.gov/infectioncontrol/guidelines/disinfection/
[3] https://www.asge.org/home/guidelines-position-statements/guidelines-for-reprocessing-gi-flexible-endoscopes
[4] https://www.apsf.org/article/bronchoscope-cleaning-and-sterilization-update/
[5] https://www.aami.org/standards
[6] https://www.hopkinsmedicine.org/infection-control/resources/endoscope-reprocessing.html
[7] https://www.sciencedirect.com/science/article/pii/S0196655319303856